Quick Answer
Anesthesia anxiety is one of the most common concerns pet owners have before surgery. This guide demystifies modern veterinary anesthesia — explaining the pre-anesthetic evaluation, how anesthetic agents work, the critical role of monitoring, what recovery looks like, and the real risk numbers. Informed owners make better decisions and experience less fear.
Key Takeaways
- ✓Anesthesia mortality in healthy dogs is ~1 in 1,849 and ~1 in 895 in cats — genuinely low in healthy patients
- ✓Underlying disease dramatically increases anesthetic risk — pre-anesthetic workup and patient optimization are critical
- ✓Continuous multi-parameter monitoring (SpO₂, EtCO₂, blood pressure, ECG, temperature) is the foundation of anesthesia safety
- ✓Hypothermia and hypotension are the most common anesthetic complications and are proactively managed
- ✓The recovery period is high-risk — dedicated monitoring until full consciousness is essential
How Safe Is Veterinary Anesthesia — The Real Numbers
Anesthesia-related mortality is one of the most common owner concerns before veterinary procedures, yet the actual risk in healthy pets is remarkably low. Understanding the real numbers helps owners make well-informed decisions rather than decisions driven by disproportionate fear.
Anesthesia Mortality in Healthy Dogs and Cats
A landmark multi-center study published in Veterinary Anaesthesia and Analgesia (the CEPSAF study) assessed anesthesia-related deaths across the UK:
- Healthy dogs: approximately 1 in 1,849 anesthetic events resulted in death
- Healthy cats: approximately 1 in 895 anesthetic events resulted in death
- Sick dogs: approximately 1 in 75 — a dramatically higher risk
- Sick cats: approximately 1 in 71
These numbers emphasize two important points: anesthesia in healthy pets is genuinely quite safe, and underlying disease dramatically increases risk. This is why pre-anesthetic assessment and optimization of the patient's condition before elective procedures significantly improves outcomes.
Context: Comparison to Human Anesthesia
For comparison, human anesthesia-related mortality in developed countries is approximately 1 in 100,000–200,000 for healthy patients undergoing elective procedures. Veterinary anesthesia risk, while higher, has improved dramatically over the past two decades as monitoring standards, drug protocols, and training have advanced.
What the Risk Is Not
Anesthesia risk is not binary — it is not "safe" versus "dangerous." Risk is a continuum influenced by patient health, the procedure performed, the duration of anesthesia, the anesthetic protocol chosen, the monitoring available, and the experience of the team. An elective dental cleaning in a healthy 3-year-old dog carries very different risk from emergency abdominal surgery in a 14-year-old dog with cardiac disease.

Pre-Anesthetic Evaluation — What Happens Before Anesthesia
The pre-anesthetic evaluation is the most important step in anesthesia safety. Its goal is to identify conditions that increase anesthetic risk and either optimize them before proceeding or adjust the anesthetic protocol accordingly.
Physical Examination
A thorough physical exam assesses:
- Cardiovascular: heart rate, rhythm, murmurs (a newly detected murmur before a dental procedure changes the risk profile significantly)
- Respiratory: respiratory rate, effort, abnormal sounds
- Hydration and body condition
- Neurological status
- Any lesions that might affect drug metabolism (liver, kidney disease)
Pre-Anesthetic Bloodwork
Bloodwork before anesthesia identifies occult disease not apparent on exam. What is recommended depends on the patient's age and health status:
- Young, healthy pets (< 5–6 years): A minimum database — PCV/TP (packed cell volume/total protein) and one or two additional markers is reasonable for very low-risk procedures; a full chemistry panel and CBC is more comprehensive
- Middle-aged pets: CBC, chemistry panel recommended
- Senior pets (7+ years): CBC, full chemistry panel, urinalysis, thyroid screening (especially cats), and cardiac evaluation (chest x-ray, ECG, +/- echocardiogram if murmur detected)
ASA Physical Status Classification
Veterinary anesthesia uses the American Society of Anesthesiologists (ASA) classification to grade patient risk:
- ASA I: Normal, healthy patient
- ASA II: Mild systemic disease (well-controlled hypothyroidism, mild obesity)
- ASA III: Moderate systemic disease that limits activity but is not incapacitating
- ASA IV: Severe systemic disease — constant threat to life
- ASA V: Moribund patient unlikely to survive without the operation
- ASA E (emergency): Added to any category for emergency procedures
Pre-Anesthetic Fasting
The traditional fasting guideline of 8–12 hours before anesthesia (to reduce regurgitation and aspiration risk) has been refined. Most guidelines now recommend:
- Dogs: 6–8 hours for food; free access to water until 2 hours before
- Cats: 4–6 hours for food (longer fasts increase hepatic lipidosis risk and hypoglycemia risk in cats)
- Pediatric patients (< 8 weeks): 2–4 hours maximum — risk of hypoglycemia is high
- Patients with megaesophagus or regurgitation history: individual protocol needed

What Is Monitored During Anesthesia
Continuous monitoring during anesthesia is what transforms anesthesia from dangerous to safe. The ACVAA (American College of Veterinary Anesthesia and Analgesia) publishes monitoring guidelines that define the standard of care.
Essential Monitoring Parameters
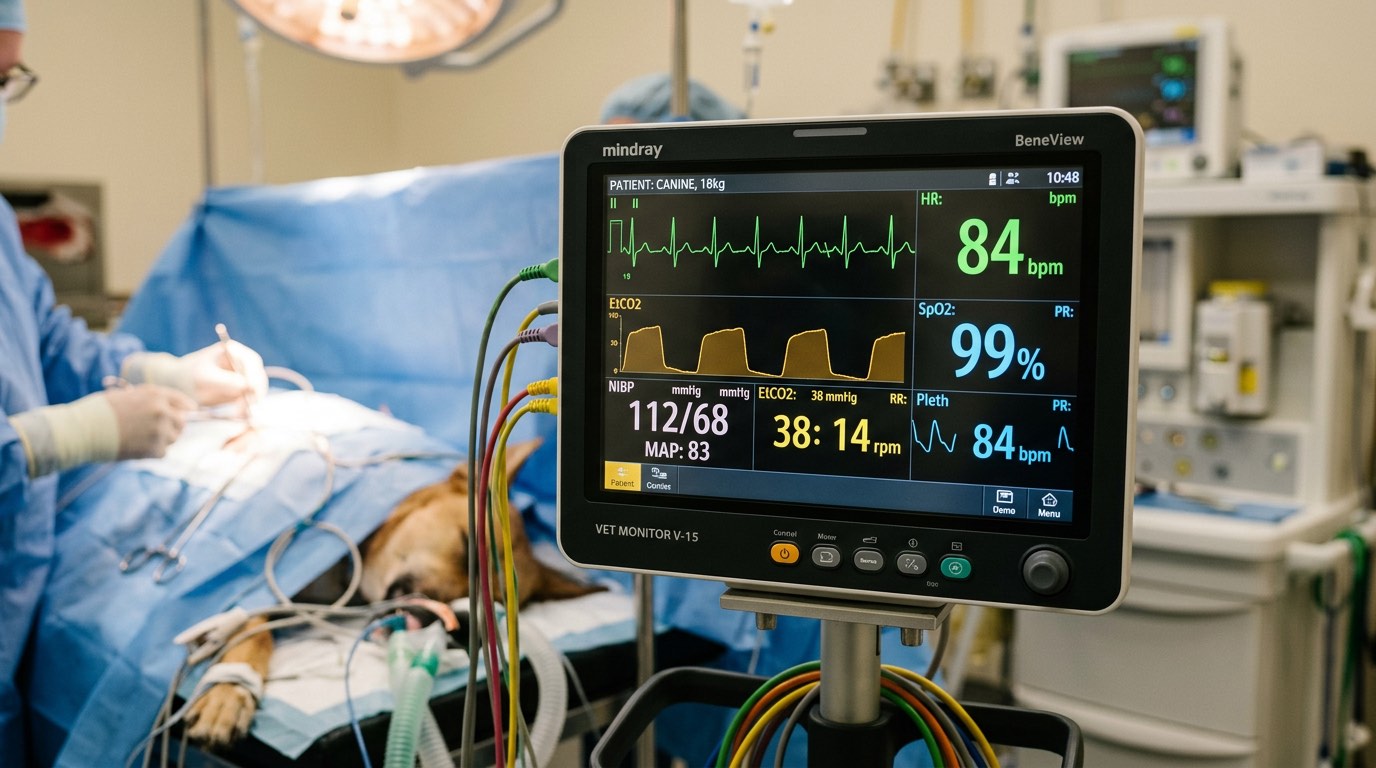
- Pulse oximetry (SpO₂): Measures the oxygen saturation of hemoglobin — the most basic measure of oxygenation. Normal is > 95%. Values below 90% require immediate intervention.
- End-tidal CO₂ (EtCO₂) / Capnography: Measures exhaled carbon dioxide, which reflects the effectiveness of ventilation. Normal range: 35–45 mmHg. Low values indicate over-ventilation or poor cardiac output; high values indicate hypoventilation. Capnography also confirms endotracheal tube placement in the trachea (not the esophagus).
- Blood pressure: Non-invasive oscillometric monitoring (like a cuff, used on limbs or tail base) or Doppler. Hypotension (mean arterial pressure < 60–65 mmHg) is the most common anesthetic complication and causes reduced tissue perfusion. It is managed with IV fluid rate adjustments, reducing anesthetic depth, and vasopressors (dopamine, dobutamine) if needed.
- Electrocardiography (ECG): Continuous heart rate and rhythm monitoring. Anesthetic agents can cause bradycardia, tachycardia, and arrhythmias — all of which can be identified and managed.
- Body temperature: Hypothermia is extremely common under anesthesia — patients lose heat rapidly through the body wall and respiratory tract. Hypothermia impairs drug metabolism, prolongs recovery, increases bleeding tendency, and impairs immune function. Active warming (forced-air warming blankets, circulating warm water blankets) is standard care.
- Depth of anesthesia assessment: Eye position, jaw tone, mucous membrane color, response to stimulation — clinical indicators of anesthetic depth.
Veterinary Technician / Anesthetist Role
Dedicated anesthesia monitoring by a trained veterinary technician or licensed veterinary technician anesthetist is a major safety factor. Having someone whose only job is to watch the patient and the monitors — rather than the surgeon also managing anesthesia — significantly improves complication detection and response times.
Recovery and How to Reduce Your Pet's Anesthetic Risk
What to Expect During Recovery
The anesthetic recovery period — from discontinuation of anesthetic agents until the patient is fully awake and able to maintain their airway — is one of the highest-risk phases of anesthesia. Most anesthesia-related deaths occur in the recovery period.
During recovery:
- The endotracheal tube is maintained until the patient is swallowing reflexes return (removed sooner in cats due to laryngospasm risk — cats are extubated at the first swallowing reflex; dogs are kept intubated longer)
- Temperature continues to be monitored and supported
- Pain assessment and analgesic administration are critical — an animal in pain has elevated stress hormones, impaired healing, and may thrash dangerously
- Quiet, warm recovery environment reduces stress and oxygen demand
Signs of Normal Recovery
- Gradual return of consciousness: moving limbs, attempting to lift head
- Return of swallowing reflex
- Chewing on endotracheal tube (dogs) — indicates it's time to remove the tube
- Shivering — common due to hypothermia, managed with warming
- Vocalization — common in cats, especially after opioids (dysphoric reaction); also common post-spay
Red Flags During Recovery
- Prolonged failure to wake up
- Respiratory distress or gasping
- Pale or blue gums
- Uncontrolled bleeding from surgical site
- Seizures
How Owners Can Reduce Anesthetic Risk
- Disclose all medications — including supplements, herbal remedies, and non-prescription drugs. Many interact with anesthetic agents.
- Disclose any prior anesthetic reactions — including prolonged recovery, arrhythmias, or malignant hyperthermia history
- Optimize pre-existing conditions: If your pet has a heart murmur, poorly controlled diabetes, or a respiratory condition, discuss stabilization before elective procedures
- Follow fasting instructions carefully
- Choose an AAHA-accredited hospital — accreditation requires documented anesthesia monitoring standards
- Ask about monitoring: It is entirely appropriate to ask your clinic what monitoring equipment they use and whether a dedicated technician monitors your pet throughout the procedure

Frequently Asked Questions
Is anesthesia safe for older dogs and cats?
Age itself is not the risk factor — underlying disease is. Many geriatric pets safely undergo anesthesia when properly evaluated and monitored. A comprehensive pre-anesthetic workup (bloodwork, urinalysis, cardiac evaluation) identifies the conditions that actually drive risk in older patients — kidney disease, cardiac disease, hypertension, anemia. Knowing what you're working with allows the anesthetic protocol to be tailored accordingly.
My vet is recommending bloodwork before a simple dental procedure. Is it really necessary?
Pre-anesthetic bloodwork provides genuinely useful information, particularly in pets over 5–6 years. Subclinical kidney disease, liver dysfunction, and anemia are not apparent on physical exam but significantly affect how anesthetic drugs are metabolized and how the kidneys handle anesthetic-related blood pressure changes. The cost of bloodwork is small relative to the value of the information — and it helps the veterinarian tailor the anesthetic protocol to your pet's specific needs.
Can my pet have anesthesia if they have a heart murmur?
Often yes — a heart murmur does not automatically preclude anesthesia. The critical questions are: what grade is the murmur? Is the underlying heart disease compensated or in failure? Has the patient been evaluated by a cardiologist? Mild, compensated murmurs in otherwise healthy dogs can be managed safely with an appropriate protocol and careful monitoring. Patients with active congestive heart failure require stabilization before elective procedures. A cardiology consultation and echocardiogram are often warranted before anesthesia in patients with moderate to severe murmurs.
What is malignant hyperthermia in pets?
Malignant hyperthermia (MH) is a rare but life-threatening genetic disorder in which volatile anesthetic agents (halothane, isoflurane, sevoflurane) trigger an uncontrolled, rapid elevation of body temperature from runaway skeletal muscle metabolism. MH is most recognized in certain pig breeds and has been reported in dogs. It is managed by immediately discontinuing the triggering agent and administering dantrolene. If a first-degree relative of your pet has experienced MH, inform your veterinarian before any procedure.
References
- Brodbelt DC, et al. "The risk of death: the confidential enquiry into perioperative small animal fatalities." Vet Anaesth Analg. 2008;35(5):365-373.
- ACVAA. "Recommendations for Monitoring of Anesthetized Veterinary Patients." American College of Veterinary Anesthesia and Analgesia. 2009.
- Grubb T, et al. "2020 WSAVA Guidelines for the Recognition, Assessment and Treatment of Pain." J Small Anim Pract. 2020.
