Quick Answer
Dental disease is the most common clinical condition in adult dogs and cats, with the majority of pets showing signs of periodontal disease by age three. This guide covers the four stages of periodontal disease, explains why professional dental cleanings under anesthesia are the gold standard of care, highlights feline odontoclastic resorptive lesions (FORLs) unique to cats, and provides actionable home dental care strategies to keep your pet's mouth healthy between veterinary visits.
Key Takeaways
- ✓Periodontal disease affects the majority of dogs and cats by age three and progresses through four stages, with only Stage 1 (gingivitis) being fully reversible.
- ✓Professional dental cleanings under general anesthesia with full-mouth radiographs are the gold standard — "anesthesia-free" cleanings cannot address disease below the gumline.
- ✓Feline odontoclastic resorptive lesions (FORLs) affect up to 70% of cats and can only be reliably diagnosed with dental radiographs during professional cleanings.
- ✓Daily tooth brushing with pet-safe toothpaste is the most effective home care strategy, supplemented by VOHC-approved dental chews, diets, and water additives.
- ✓Watch for warning signs such as bad breath, red gums, difficulty eating, or behavioral changes, and schedule a veterinary dental evaluation promptly if any are observed.
Understanding Periodontal Disease in Pets
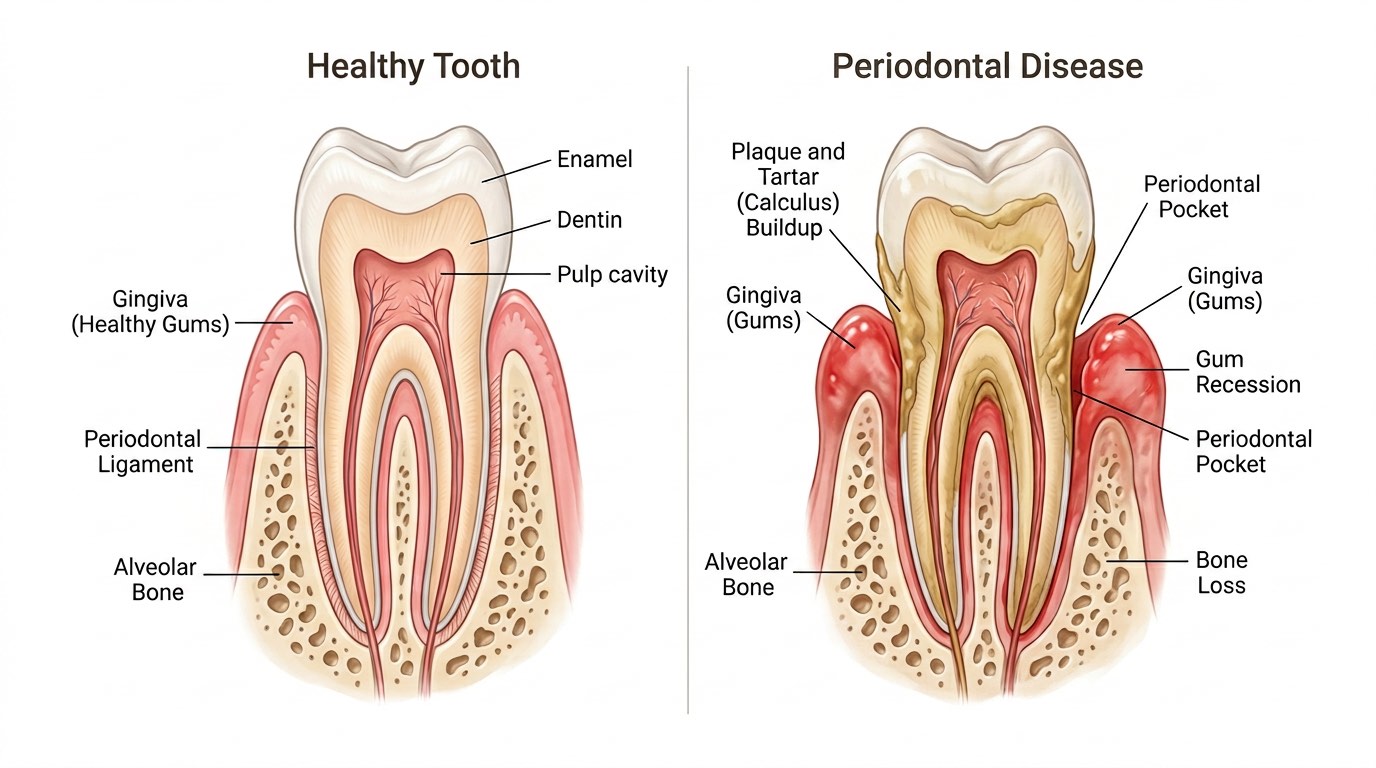
Periodontal disease is a progressive inflammatory condition affecting the structures that support the teeth — the gingiva (gums), periodontal ligament, cementum, and alveolar bone — and it is estimated that over 80 percent of dogs and 70 percent of cats have some degree of dental disease by the age of three. The process begins when bacteria in the mouth form a sticky biofilm called plaque on the tooth surface, which mineralizes into tartar (calculus) within 72 hours if not removed. As plaque and tartar accumulate along and beneath the gumline, they trigger an immune-mediated inflammatory response that damages the soft tissue attachment and, over time, erodes the underlying bone. Unlike cavities in humans, which are relatively uncommon in pets, periodontal disease is the primary dental threat and can lead to tooth loss, chronic pain, difficulty eating, and bacteremia that may affect the heart, liver, and kidneys. Early intervention is key because the earliest stages of periodontal disease are reversible, while advanced stages cause irreversible damage that can only be managed, not cured.
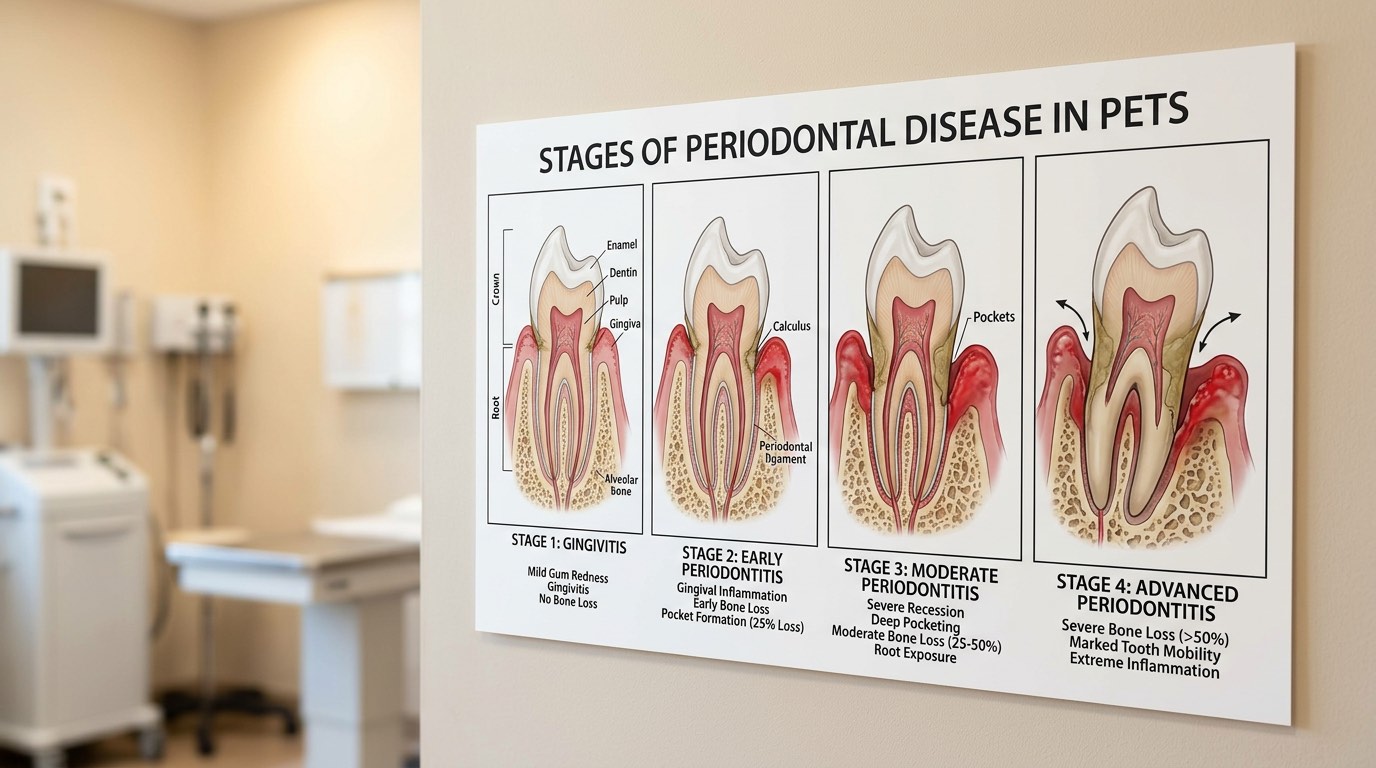
The Four Stages of Periodontal Disease
Veterinary dentists classify periodontal disease into four stages based on the degree of tissue damage, and understanding these stages helps you appreciate why early detection matters so much. Stage 1 (gingivitis) is the only fully reversible stage and is characterized by reddened, swollen gums that may bleed easily when probed, but with no loss of attachment or bone — a thorough professional cleaning and consistent home care can completely resolve it. Stage 2 (early periodontitis) involves up to 25 percent loss of the tooth's supporting attachment, meaning the periodontal ligament and bone are beginning to break down; dental radiographs are essential at this point because damage beneath the gumline is invisible to the naked eye. Stage 3 (moderate periodontitis) features 25 to 50 percent attachment loss, deeper periodontal pockets, and often visible gum recession or tooth mobility, and while some teeth can be saved with advanced periodontal treatments, extractions may be necessary for severely affected teeth. Stage 4 (severe periodontitis) involves greater than 50 percent attachment loss with significant bone destruction, tooth root exposure, and loose or painful teeth that almost always require extraction to eliminate chronic infection and restore comfort.
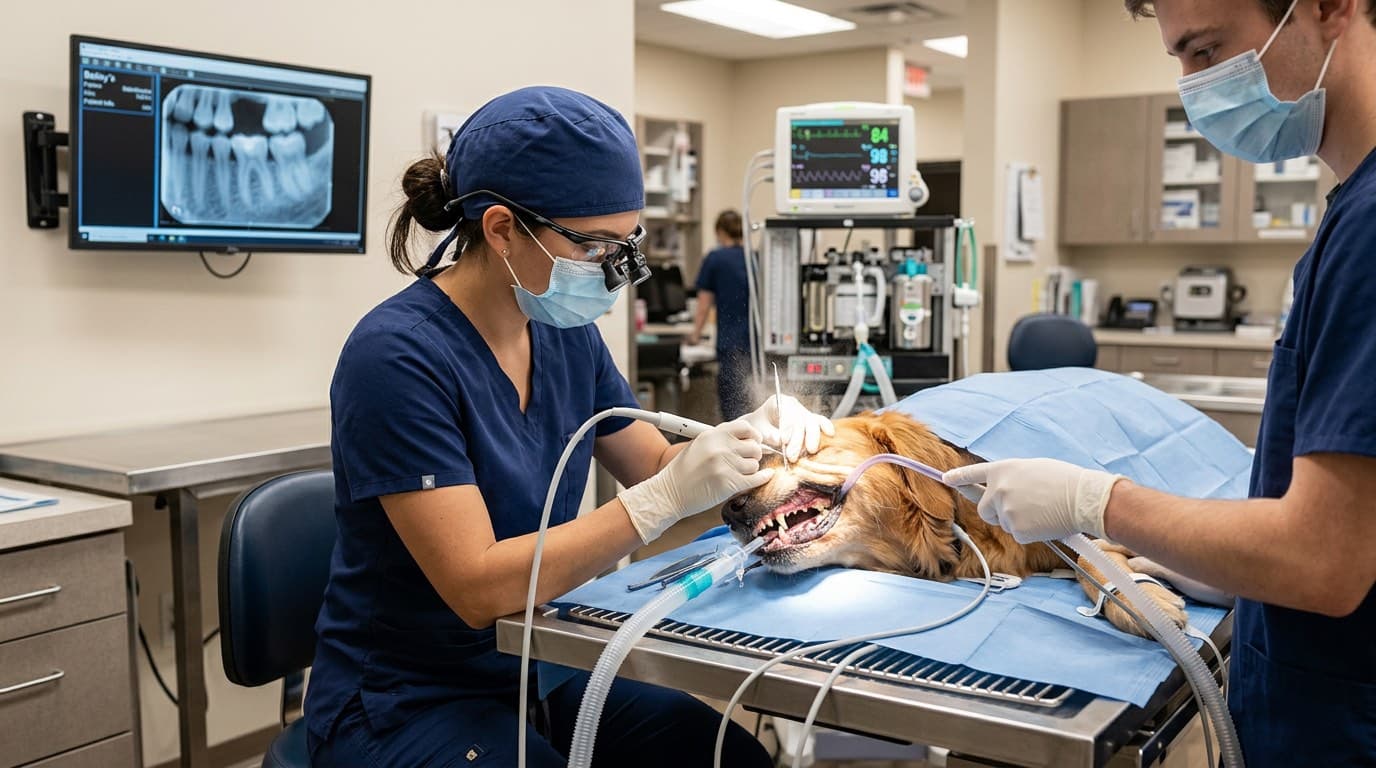
Professional Dental Cleaning Under Anesthesia
A professional veterinary dental cleaning, formally called a comprehensive oral health assessment and treatment (COHAT), requires general anesthesia because a thorough examination and cleaning of every tooth surface — including those below the gumline — is impossible in an awake patient. During the procedure, the veterinary team performs a complete oral examination, charts each tooth, takes full-mouth dental radiographs to evaluate the roots and surrounding bone, and uses an ultrasonic scaler to remove plaque and tartar from all surfaces above and below the gumline. Each tooth is then polished to smooth microscopic etchings left by the scaler, which slows the reaccumulation of plaque, and fluoride or a dental sealant may be applied. If dental radiographs reveal diseased teeth with advanced attachment loss, root abscesses, or fractured roots, extractions are performed during the same anesthetic event using nerve blocks for pain control. So-called "anesthesia-free" dental cleanings are strongly discouraged by the American Veterinary Dental College because they only address visible tartar above the gumline, cannot treat subgingival disease, and often create a false sense of security while the real disease progresses unseen.
Feline Odontoclastic Resorptive Lesions (FORLs)
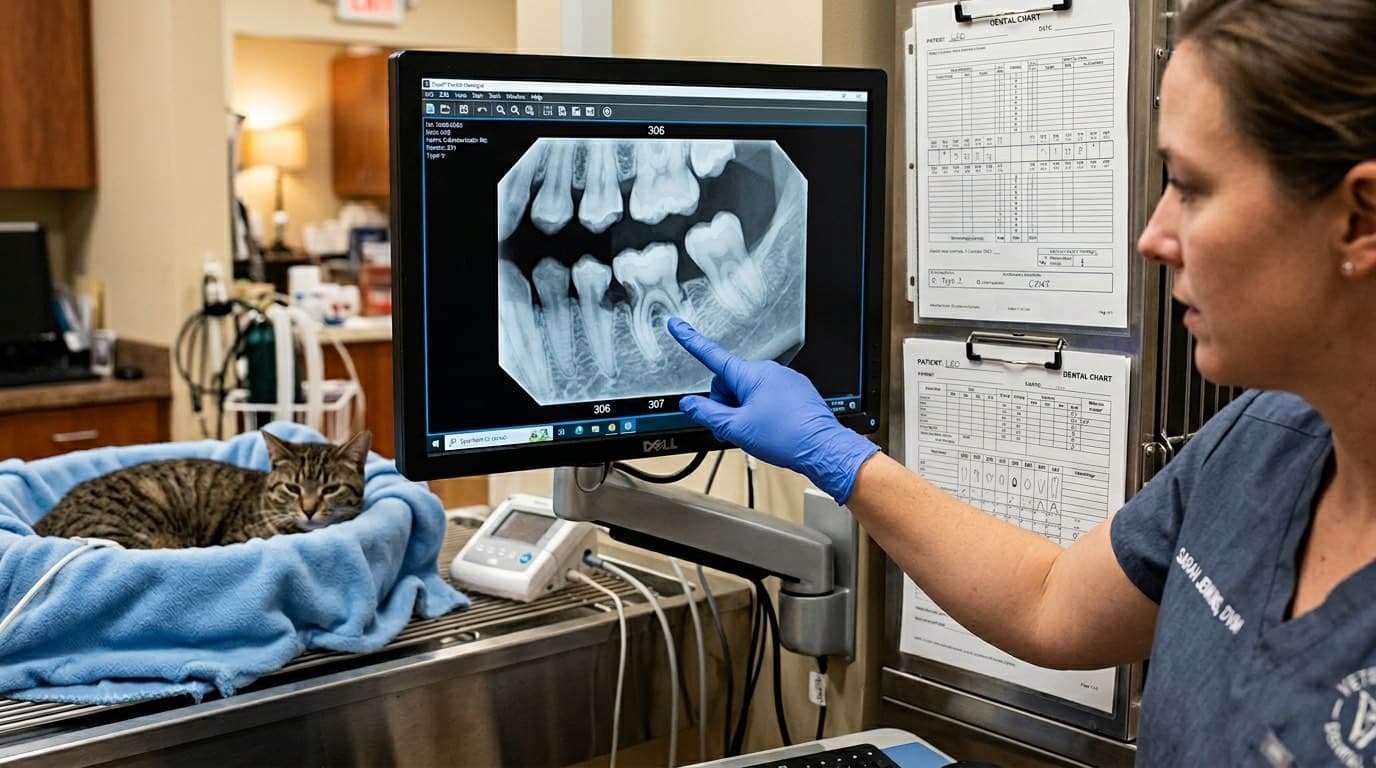
Feline odontoclastic resorptive lesions, commonly known as FORLs or tooth resorption, are a painful and prevalent dental condition affecting an estimated 30 to 70 percent of cats, with incidence increasing with age. FORLs occur when cells called odontoclasts begin to erode and destroy the tooth structure itself — starting at the root surface or at the cementoenamel junction — causing progressive loss of tooth integrity that is distinct from periodontal disease. Cats with FORLs may show signs of oral pain such as difficulty eating, dropping food, head shaking, excessive drooling, or jaw chattering, though many cats hide their discomfort remarkably well. Dental radiographs are indispensable for diagnosing and classifying FORLs: Type 1 lesions show resorption with a normal-appearing root, requiring extraction of the entire tooth, while Type 2 lesions involve replacement of the root by bone (ghost roots) and may be treated with crown amputation. The exact cause of FORLs remains unknown despite extensive research, and no proven preventive strategy exists, making routine dental radiographs during professional cleanings the most reliable way to catch and treat these painful lesions early.
What You Can Do at Home
Daily tooth brushing is the single most effective home dental care strategy, and with patience and positive reinforcement, most dogs and many cats can learn to accept it as part of their routine. Use a pet-specific toothpaste — never human toothpaste, which contains fluoride and xylitol that are toxic to pets — and a soft-bristled finger brush or small pet toothbrush, focusing on the outer surfaces of the teeth where plaque accumulates most heavily. If your pet will not tolerate brushing, veterinary-approved dental chews, water additives, and dental diets carrying the Veterinary Oral Health Council (VOHC) seal of acceptance provide supplemental plaque control, though they are not a substitute for brushing or professional cleanings. Make it a habit to regularly lift your pet's lips and look at their teeth and gums; healthy gums should be pink and firm, and you should watch for redness, swelling, bleeding, broken teeth, or persistent bad breath that goes beyond normal "doggy breath." Starting dental care when your pet is young sets the foundation for a lifetime of better oral health, but it is never too late to begin — even senior pets benefit enormously from a professional cleaning followed by consistent home care.

When to See Your Veterinarian
Schedule a dental evaluation if you notice persistent bad breath, red or bleeding gums, visible tartar buildup, loose or discolored teeth, drooling, pawing at the mouth, or any change in eating habits such as favoring one side, dropping food, or reluctance to eat hard kibble. Cats can be particularly subtle about oral pain, so behavioral changes like hiding more, becoming irritable when touched around the head, or grooming less frequently may be the only clues that a dental problem exists. Your veterinarian should perform an oral assessment as part of every annual wellness exam, but pets with a history of dental disease or breeds predisposed to dental problems — such as Greyhounds, small-breed dogs, and Siamese cats — may benefit from more frequent evaluations. Do not attempt to remove tartar at home with metal instruments, as you risk damaging the enamel, injuring the gums, or pushing bacteria deeper beneath the gumline. A timely professional dental cleaning can prevent the need for costly extractions later and, most importantly, eliminates a source of chronic pain and infection that significantly impacts your pet's overall well-being.

Frequently Asked Questions
Why does my pet need to be under anesthesia for a dental cleaning?
General anesthesia is necessary to perform a thorough cleaning below the gumline, take diagnostic dental radiographs, and safely examine every tooth in the mouth — none of which can be done properly on an awake patient. Anesthesia also protects your pet's airway with an endotracheal tube, preventing water and debris from entering the lungs during the procedure. Modern veterinary anesthesia with pre-anesthetic blood work and continuous monitoring is very safe, even for older pets.
How often should my dog or cat have a professional dental cleaning?
The frequency depends on your individual pet's oral health, breed predisposition, and how effectively you manage home dental care. Many pets benefit from annual dental cleanings, while some small-breed dogs or cats prone to dental disease may need cleanings every six to twelve months. Your veterinarian will recommend a schedule based on the findings at each oral assessment and how quickly plaque and tartar reaccumulate.
What are FORLs and how do I know if my cat has them?
Feline odontoclastic resorptive lesions (FORLs) are a painful condition in which a cat's own cells gradually destroy the tooth structure, affecting an estimated 30 to 70 percent of cats. Because cats are experts at hiding pain, you may not notice obvious signs, though some cats show jaw chattering, drooling, or reluctance to eat. The only reliable way to diagnose FORLs is through dental radiographs taken during a professional dental cleaning under anesthesia.
Is it safe to brush my cat's teeth, and how do I start?
Yes, it is safe and beneficial to brush your cat's teeth, though it requires a gradual, positive introduction over several weeks. Start by letting your cat lick a small amount of pet-safe toothpaste from your finger, then progress to gently rubbing the paste along the gumline with your finger before introducing a finger brush. Keep sessions short (under 30 seconds initially), reward your cat afterward, and be patient — consistency and positive association are more important than perfection.
Can dental disease really affect my pet's heart, kidneys, and liver?
Yes, chronic periodontal disease creates a persistent source of bacteria that can enter the bloodstream through inflamed gum tissue, a process called bacteremia. Research has demonstrated associations between severe periodontal disease and microscopic changes in the heart, liver, and kidneys of dogs. While the exact degree of systemic impact is still being studied, maintaining good oral health is widely recognized by veterinary professionals as an important component of overall wellness and disease prevention.
References
- American Veterinary Dental College — "Companion Animal Dental Scaling Without Anesthesia." Position statement available at: avdc.org.
- Bellows, J. et al. (2019). "2019 AAHA Dental Care Guidelines for Dogs and Cats." Journal of the American Animal Hospital Association, 55(2), 49-69.
- Merck Veterinary Manual — "Periodontal Disease in Small Animals." Available at: merckvetmanual.com.
- Cornell University College of Veterinary Medicine — "Feline Dental Disease." Available at: vet.cornell.edu.