Quick Answer
A comprehensive veterinary guide to diabetes mellitus in dogs and cats, covering clinical signs, diagnosis, insulin therapy, blood glucose monitoring, dietary management, diabetic ketoacidosis, and practical home care strategies for long-term glycemic control.
Key Takeaways
- ✓Diabetes mellitus causes persistent high blood glucose due to insulin deficiency (dogs, Type 1) or insulin resistance (cats, Type 2), and is highly manageable with consistent treatment
- ✓The classic signs are increased thirst, urination, appetite, and weight loss — early recognition leads to better outcomes
- ✓Insulin therapy paired with consistent meals and regular glucose monitoring is the cornerstone of treatment for both species
- ✓Diabetic ketoacidosis (DKA) is a life-threatening emergency that requires immediate hospitalization and aggressive treatment
- ✓Up to 30% of diabetic cats can achieve remission with early insulin therapy, a low-carbohydrate diet, and weight management
What Is Diabetes Mellitus?
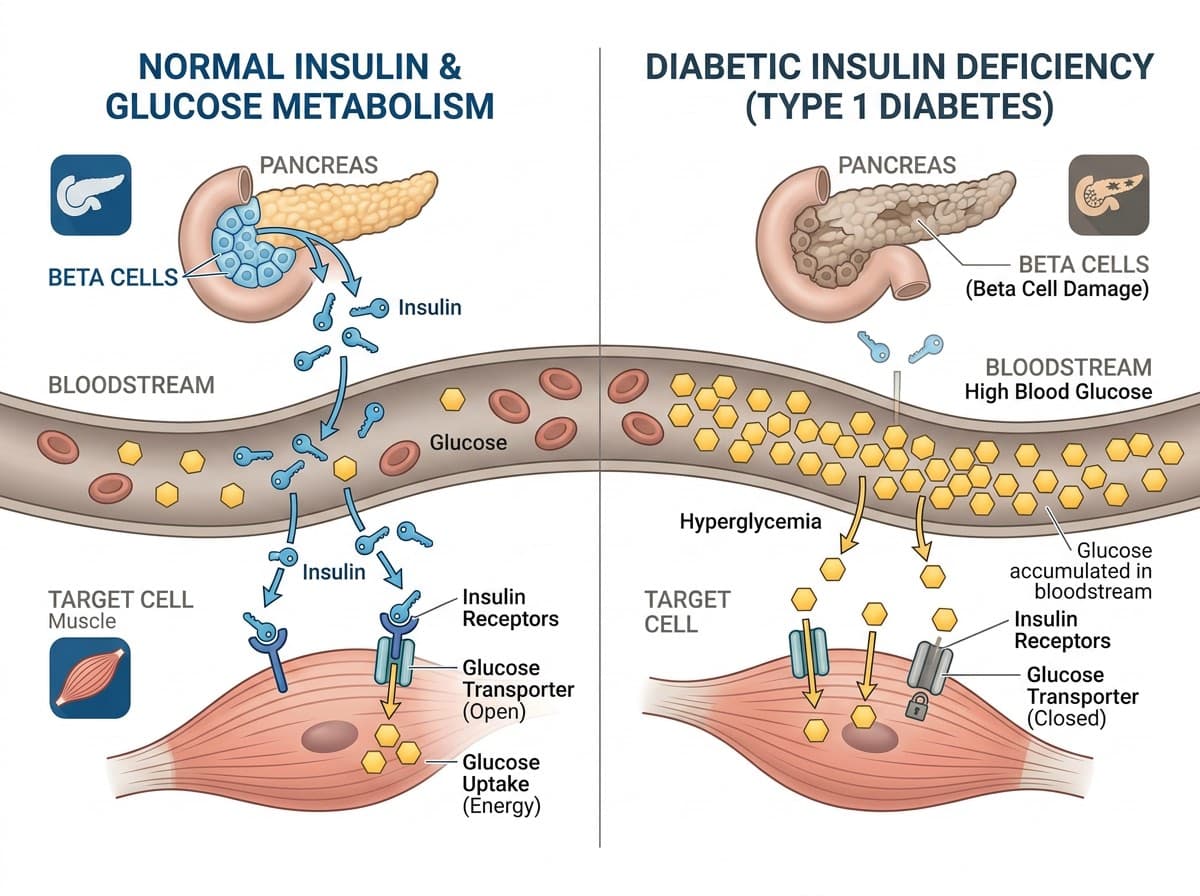
Diabetes mellitus is a chronic endocrine disorder in which the body either cannot produce enough insulin or cannot use insulin effectively, resulting in persistently elevated blood glucose (hyperglycemia). In dogs, the disease is most commonly Type 1 — the insulin-producing beta cells of the pancreas are destroyed by immune-mediated processes, and the dog becomes permanently dependent on exogenous insulin. In cats, Type 2 diabetes predominates, characterized by a combination of insulin resistance and impaired beta-cell function, often associated with obesity and sedentary lifestyle.
Diabetes is among the most frequently diagnosed endocrine diseases in companion animals, and its prevalence has been increasing in parallel with rising obesity rates. Certain breeds carry higher risk: Samoyeds, Australian Terriers, Miniature Schnauzers, and Poodles in dogs; Burmese cats have a well-documented genetic predisposition. Middle-aged to older animals are most commonly affected, with unspayed female dogs and neutered male cats at particularly elevated risk.
The good news is that diabetes, while incurable in most dogs, is highly manageable with consistent insulin therapy, dietary modification, and regular monitoring. In cats, early and aggressive treatment can sometimes achieve diabetic remission — a state where the cat maintains normal blood glucose without insulin — making prompt diagnosis and treatment especially important in feline patients.
Recognizing the Signs and Getting a Diagnosis
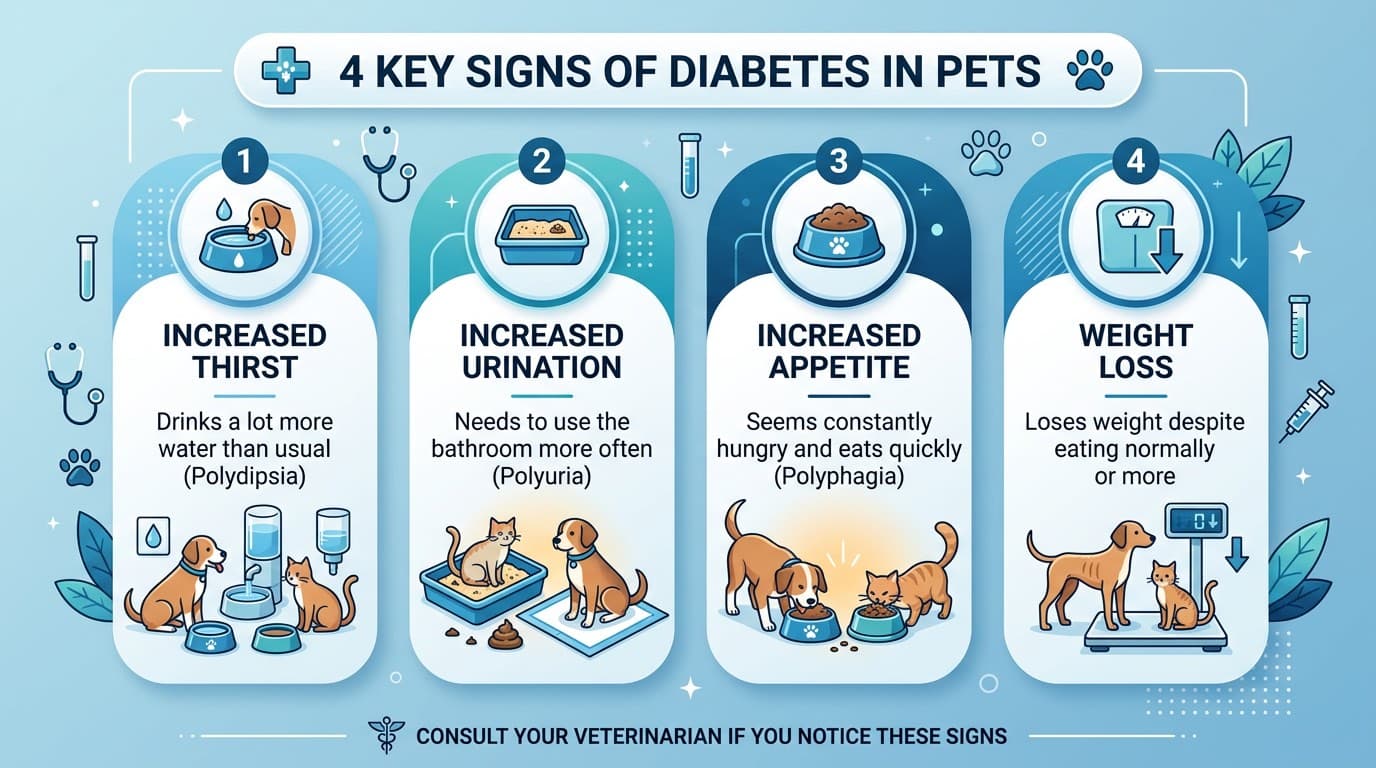
The classic clinical signs of diabetes mellitus are often referred to as the "four Ps": polyuria (excessive urination), polydipsia (excessive drinking), polyphagia (increased appetite), and paradoxical weight loss despite eating more. These signs develop because glucose cannot enter cells efficiently without adequate insulin, so the body breaks down fat and muscle for energy while excess glucose spills into the urine and pulls water with it. Owners frequently notice that they are refilling the water bowl more often, the litter box is soggier than usual, or the dog is urinating in the house despite being previously house-trained.
If left untreated, diabetes progresses to more severe complications. Dogs may develop cataracts — often rapidly — leading to noticeable cloudiness in the eyes and vision loss. Cats may develop a characteristic plantigrade stance, walking on their hocks rather than their toes, due to diabetic neuropathy affecting the hind limbs. Both species may become lethargic, develop recurrent urinary tract infections, and show poor wound healing as hyperglycemia impairs immune function.
Diagnosis requires demonstrating persistent fasting hyperglycemia combined with glucosuria (glucose in the urine). A single elevated blood glucose reading is not sufficient in cats, because stress hyperglycemia is common during veterinary visits and can be misleading. Fructosamine levels — which reflect average blood glucose over the preceding two to three weeks — help distinguish true diabetes from transient stress-related elevations. A complete blood panel, urinalysis, and urine culture are typically performed to screen for concurrent conditions such as urinary tract infections, pancreatitis, or Cushing's disease in dogs.
Insulin Therapy and Blood Glucose Monitoring
Insulin therapy is the foundation of diabetes management in both dogs and cats. The specific insulin type, dose, and injection frequency are tailored to the individual patient. Dogs are most commonly started on intermediate-acting insulins such as Vetsulin (porcine lente insulin) or NPH insulin, typically administered twice daily with meals. Cats often respond well to longer-acting insulins such as glargine (Lantus) or protamine zinc insulin (ProZinc), which provide more stable glucose control and a higher chance of achieving remission.
The initial insulin dose is a starting point that will be refined over the following weeks through glucose monitoring. Blood glucose curves — serial measurements taken every two to four hours over a full day — reveal how the insulin is affecting glucose levels over its duration of action. These curves help the veterinarian identify the glucose nadir (lowest point), duration of effect, and appropriate dose adjustments. Some clinics now use continuous glucose monitors (CGMs) such as the FreeStyle Libre, which can be applied to a pet's skin and provide real-time glucose readings without repeated needle sticks.
Owners must become comfortable with drawing up and administering subcutaneous insulin injections, which are given using small insulin syringes or pen devices. The injection is typically given in the scruff of the neck or along the side of the body, rotating sites to prevent lipodystrophy. Consistent timing is critical — insulin should be given at the same times each day, always with a meal, to prevent dangerous hypoglycemic episodes. Hypoglycemia (blood glucose below 60 mg/dL) is the most serious acute risk of insulin therapy and can cause weakness, trembling, disorientation, seizures, or collapse if not recognized and treated promptly with oral sugar solution.

Diabetic Ketoacidosis: A Life-Threatening Emergency
Diabetic ketoacidosis (DKA) is the most dangerous acute complication of diabetes mellitus and constitutes a genuine veterinary emergency. DKA occurs when the body, starved of usable glucose due to insulin deficiency, breaks down fat at an accelerated rate, producing ketone bodies (acetoacetate, beta-hydroxybutyrate, and acetone) that accumulate in the blood and cause a severe metabolic acidosis. DKA can develop in undiagnosed diabetics or in known diabetic patients who miss insulin doses, develop a concurrent illness, or experience a sudden increase in insulin resistance.
Clinical signs of DKA include profound lethargy, vomiting, diarrhea, complete loss of appetite, dehydration, rapid or labored breathing (Kussmaul respiration as the body attempts to compensate for acidosis), and a fruity or acetone-like odor on the breath. Affected pets may become weak, collapse, or become obtunded. Without aggressive treatment, DKA progresses to multi-organ failure and death within hours to days.
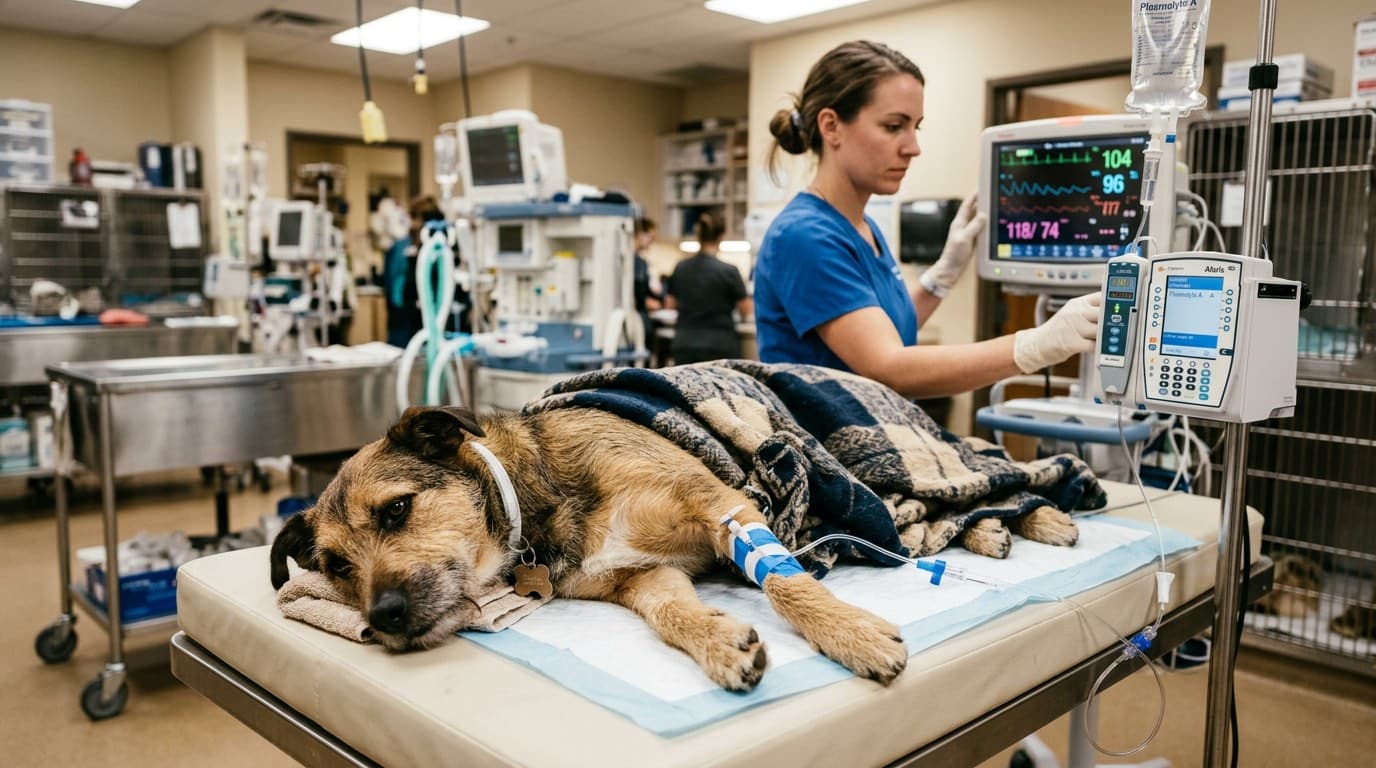
Treatment requires hospitalization with intravenous fluid therapy to correct dehydration and electrolyte imbalances, regular-acting insulin administered intravenously or intramuscularly to gradually lower blood glucose and halt ketone production, careful potassium supplementation (insulin drives potassium into cells, which can cause dangerous hypokalemia), and identification and treatment of any underlying trigger such as infection, pancreatitis, or urinary obstruction. The survival rate for DKA with aggressive treatment is approximately 70%, underscoring the importance of preventing episodes through consistent insulin therapy and early recognition of warning signs.
What You Can Do at Home
Successful diabetes management depends heavily on the owner's commitment to a consistent daily routine. Feeding the same measured meals at the same times each day — always paired with insulin injections — is the single most important habit to establish. For dogs, high-fiber, complex-carbohydrate diets help slow glucose absorption and improve postprandial glycemic control. For cats, high-protein, low-carbohydrate diets are recommended because they more closely match feline metabolic needs and significantly improve glycemic regulation, increasing the likelihood of remission.
Learn to recognize the signs of hypoglycemia — trembling, weakness, stumbling, glazed eyes, unresponsiveness — and keep a bottle of corn syrup or honey accessible at all times. If your pet shows signs of low blood sugar, immediately rub a small amount of syrup on the gums (do not force a seizing animal to swallow) and contact your veterinarian. Never adjust insulin doses on your own without veterinary guidance, as even small changes can have outsized effects on blood glucose.
Monitor your pet's weight weekly using a consistent scale, track daily water intake, and log appetite and energy levels. These simple observations create a longitudinal picture that helps your veterinarian make precise dose adjustments at recheck appointments. Keep insulin stored properly — most insulin should be refrigerated, gently rolled (never shaken) before use, and discarded after its expiration or recommended use-after-opening period. Maintain a written schedule for injections to avoid accidental double-dosing, especially in multi-person households where more than one family member might administer the injection.

Long-Term Outlook and Diabetic Remission
With dedicated management, many diabetic dogs and cats live full, comfortable lives for years after diagnosis. Diabetic dogs will typically require lifelong insulin therapy, but well-regulated dogs experience normal energy levels, maintain healthy weights, and enjoy their usual activities. Regular veterinary rechecks — typically every three to four months for stable patients — include blood glucose curves or fructosamine levels, complete blood panels, and urinalysis to monitor for complications.
Cats have a unique advantage: approximately 25-30% of diabetic cats achieve remission when treated early and aggressively with appropriate insulin and a low-carbohydrate diet. Remission means the cat can maintain normal blood glucose levels without insulin injections, though these cats remain at risk for relapse and should continue to be monitored. Achieving and maintaining a healthy body weight is one of the strongest predictors of remission in cats — even modest weight loss in overweight diabetic cats can dramatically improve insulin sensitivity.
Long-term complications to monitor include diabetic cataracts in dogs (which can develop rapidly and may benefit from surgical removal), diabetic neuropathy in cats (which usually improves with glycemic control), recurrent urinary tract infections, and the potential development of concurrent endocrine diseases such as Cushing's disease in dogs or hyperthyroidism in cats. A collaborative relationship between the owner and the veterinary team — built on clear communication, consistent monitoring, and realistic expectations — is the foundation of successful long-term diabetic care.

Frequently Asked Questions
What causes diabetes in dogs and cats?
In dogs, diabetes is most often caused by immune-mediated destruction of the insulin-producing beta cells of the pancreas, similar to Type 1 diabetes in humans. In cats, it is typically Type 2, driven by insulin resistance often linked to obesity, physical inactivity, and genetic factors. Pancreatitis, Cushing's disease, and long-term corticosteroid use can also trigger or worsen diabetes in both species.
Can a diabetic pet ever stop needing insulin?
Most diabetic dogs require insulin for life. However, approximately 25-30% of diabetic cats can achieve remission — meaning they no longer need insulin injections — when treated early and aggressively with appropriate insulin and a low-carbohydrate diet. Weight loss in overweight cats significantly increases the chances of remission. Even cats in remission require ongoing monitoring because relapse is possible.
How do I know if my pet is having a hypoglycemic episode?
Signs of hypoglycemia include trembling or shaking, weakness, stumbling or loss of coordination, a dazed or glassy-eyed appearance, and in severe cases, seizures or collapse. If you observe these signs, immediately rub a small amount of corn syrup or honey on your pet's gums and contact your veterinarian. Never skip a meal before an insulin injection, and never increase the insulin dose without veterinary guidance.
What should I feed a diabetic dog or cat?
For diabetic dogs, high-fiber diets with complex carbohydrates help slow glucose absorption and improve glycemic control. For diabetic cats, high-protein, low-carbohydrate diets are strongly recommended because they better match feline metabolism and significantly improve blood glucose regulation. Your veterinarian can recommend specific therapeutic diets. Consistency in feeding amounts and timing is just as important as the diet itself.
How much does it cost to treat a diabetic pet?
Costs vary depending on the type of insulin, monitoring frequency, and any complications that arise. Ongoing expenses typically include insulin, syringes, prescription food, and veterinary rechecks every three to four months. Many owners find the costs manageable once the initial stabilization period is complete. Pet insurance may cover a portion of diabetic care if the policy was in place before diagnosis.
References
- Behrend, E., et al. "2018 AAHA Diabetes Management Guidelines for Dogs and Cats." Journal of the American Animal Hospital Association, vol. 54, no. 1, 2018, pp. 1-21.
- Cornell University College of Veterinary Medicine. "Feline Diabetes." Cornell Feline Health Center, 2024.
- Merck Veterinary Manual. "Diabetes Mellitus in Dogs and Cats." Merck & Co., 2023.
- Nelson, R.W. "Canine Diabetes Mellitus." Textbook of Veterinary Internal Medicine, 8th Edition, Elsevier, 2020.
