Quick Answer
Cushing's disease (hyperadrenocorticism) is one of the most common endocrine disorders in middle-aged and older dogs. This comprehensive guide explains the difference between pituitary-dependent and adrenal-dependent forms, walks you through diagnostic testing such as the LDDS, HDDS, and ACTH stimulation test, and covers treatment options including trilostane and mitotane so you can work confidently with your veterinary team.
Key Takeaways
- ✓Cushing's disease is caused by chronic cortisol overproduction, with 80-85% of cases being pituitary-dependent (PDH) and 15-20% being adrenal-dependent (ADH).
- ✓Classic signs include increased thirst, urination, appetite, a pot-bellied appearance, hair loss, and recurrent infections — symptoms that often develop gradually.
- ✓Accurate diagnosis requires specialized endocrine tests such as the LDDS, ACTH stimulation test, or HDDS, often combined with abdominal ultrasound.
- ✓Trilostane is the most commonly used treatment and requires lifelong administration with regular ACTH stimulation monitoring to adjust dosing.
- ✓Home management success depends on medication consistency, keeping a symptom diary, attending all monitoring appointments, and watching for signs of cortisol dropping too low.
What Is Cushing's Disease?
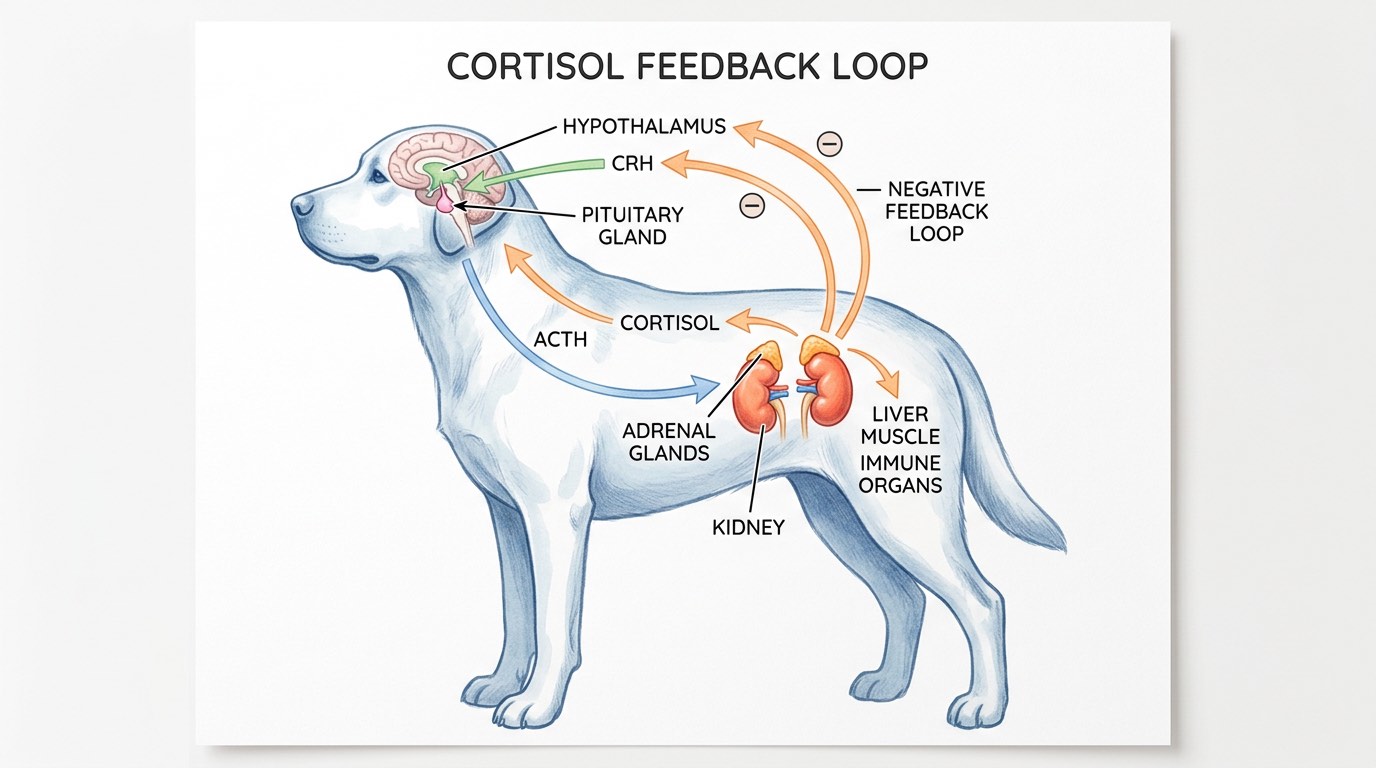
Cushing's disease, known medically as hyperadrenocorticism, occurs when a dog's body produces excessive amounts of cortisol, a steroid hormone manufactured by the adrenal glands. Cortisol plays essential roles in regulating metabolism, blood sugar, immune function, and the body's stress response, but chronic overproduction wreaks havoc on nearly every organ system. The condition most frequently affects dogs over the age of six, with breeds such as Poodles, Dachshunds, Boston Terriers, Boxers, and Beagles showing a higher predisposition. Left untreated, Cushing's disease can lead to serious secondary complications including diabetes mellitus, recurrent infections, hypertension, and thromboembolic events. Early recognition and appropriate treatment can dramatically improve quality of life, so understanding the hallmark signs is the first step toward helping your dog.
Pituitary-Dependent vs. Adrenal-Dependent Cushing's
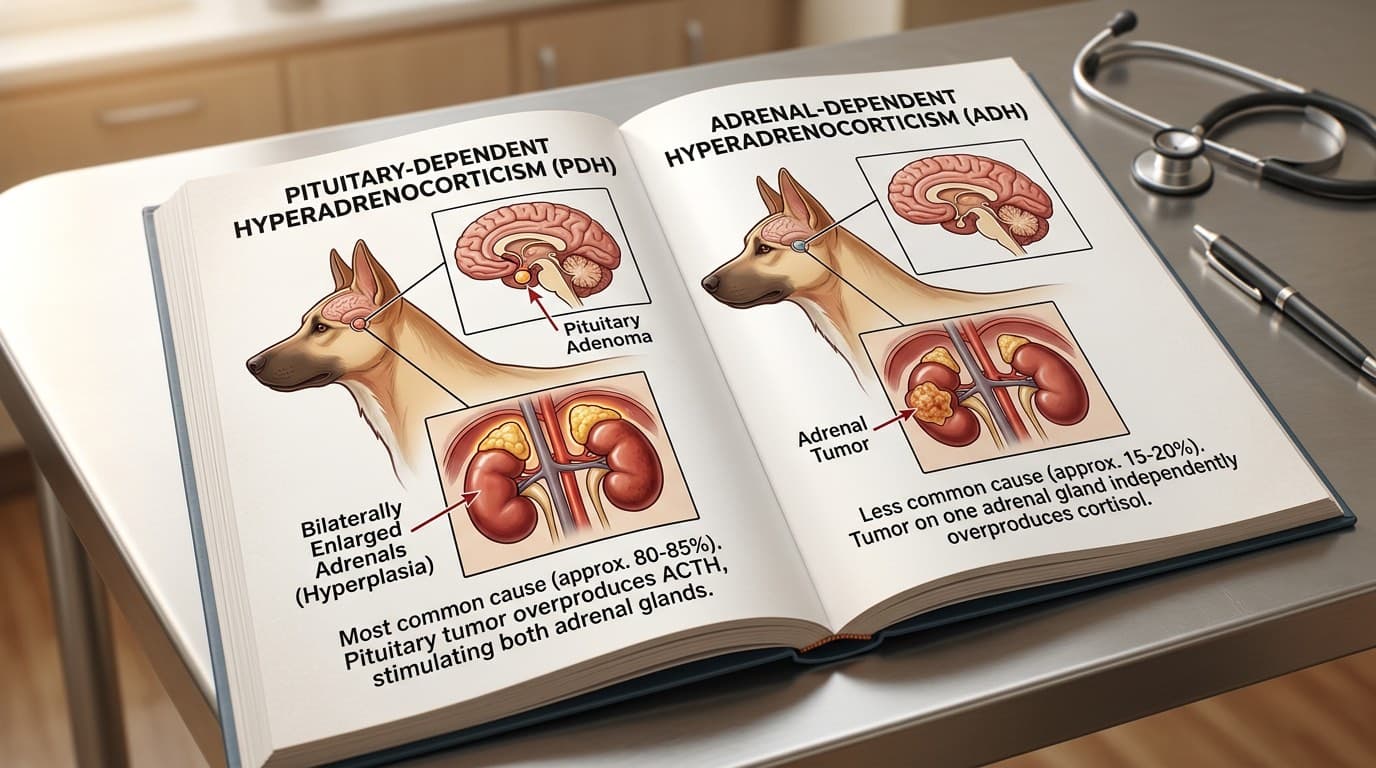
Approximately 80 to 85 percent of canine Cushing's cases are pituitary-dependent hyperadrenocorticism (PDH), caused by a benign microadenoma or, less commonly, a macroadenoma of the pituitary gland that secretes excessive adrenocorticotropic hormone (ACTH). This surplus ACTH continuously stimulates both adrenal glands, causing them to enlarge bilaterally and overproduce cortisol. The remaining 15 to 20 percent of cases are adrenal-dependent hyperadrenocorticism (ADH), resulting from a functional tumor — either an adenoma or carcinoma — on one of the adrenal glands that autonomously secretes cortisol regardless of ACTH levels. Distinguishing between PDH and ADH is clinically critical because the treatment approach and prognosis differ substantially; for example, surgical adrenalectomy may be curative for ADH while PDH typically requires lifelong medical management. Your veterinarian will use a combination of blood work, diagnostic imaging such as abdominal ultrasound, and specialized endocrine tests to determine which form your dog has.
Recognizing the Signs of Cushing's Disease
The clinical signs of Cushing's disease often develop gradually, leading many owners to attribute them to normal aging before a diagnosis is made. The most recognizable symptoms include increased thirst and urination (polydipsia and polyuria), a ravenous appetite (polyphagia), and a noticeably distended or pot-bellied abdomen caused by hepatomegaly and redistribution of body fat. Many dogs develop bilateral symmetrical hair loss, thin and fragile skin that bruises easily, and recurrent skin or urinary tract infections due to cortisol's immunosuppressive effects. You may also notice excessive panting even at rest, muscle weakness or wasting in the hind limbs, lethargy, and a reluctance to exercise or climb stairs. Because these signs overlap with other conditions such as hypothyroidism and diabetes, a thorough diagnostic workup is essential to confirm the diagnosis and rule out concurrent diseases.
Diagnostic Testing: LDDS, HDDS, and ACTH Stimulation
Diagnosing Cushing's disease requires specialized endocrine testing because routine blood work alone is suggestive but not definitive. The low-dose dexamethasone suppression test (LDDS) is often the first-line screening test; it involves administering a small dose of dexamethasone intravenously and measuring cortisol levels at four and eight hours — in a healthy dog cortisol drops significantly, whereas in a dog with Cushing's it remains elevated. The ACTH stimulation test measures how the adrenal glands respond to a synthetic ACTH injection by comparing pre- and post-injection cortisol levels, and while it is less sensitive than the LDDS for naturally occurring Cushing's, it is the preferred test for monitoring treatment response and diagnosing iatrogenic Cushing's. The high-dose dexamethasone suppression test (HDDS) is used specifically to differentiate PDH from ADH — pituitary tumors typically show partial suppression at the higher dose, while adrenal tumors do not suppress. Your veterinarian may also recommend abdominal ultrasound to visualize adrenal gland size and symmetry, advanced imaging like CT or MRI for pituitary assessment, and a urine cortisol-to-creatinine ratio as an initial screening tool.

Treatment: Trilostane, Mitotane, and Surgery
Trilostane (brand name Vetoryl) has become the most widely prescribed medical treatment for canine Cushing's disease and works by reversibly inhibiting 3-beta-hydroxysteroid dehydrogenase, an enzyme essential for cortisol synthesis in the adrenal glands. It is typically administered once or twice daily with food, and dogs require regular ACTH stimulation tests — initially every two to four weeks, then every three to six months — to fine-tune the dosage and ensure cortisol levels remain in a safe therapeutic range. Mitotane (Lysodren) is an older adrenolytic drug that selectively destroys the cortisol-producing layers of the adrenal cortex, and while effective, it carries a higher risk of serious side effects including adrenal necrosis and Addisonian crisis, so it is generally reserved for cases unresponsive to trilostane. For adrenal-dependent Cushing's caused by an operable adrenal tumor, surgical adrenalectomy performed by a board-certified veterinary surgeon can be curative, though the procedure carries perioperative risks and requires careful post-operative monitoring for cortisol withdrawal. Regardless of the treatment chosen, lifelong monitoring is essential, and you should watch for warning signs such as vomiting, diarrhea, lethargy, or collapse, which may indicate the cortisol level has dropped too low.

What You Can Do at Home
Managing a dog with Cushing's disease at home begins with strict medication compliance — give trilostane or mitotane at the same time each day with a meal, and never skip or double doses without consulting your veterinarian. Keep a daily log of your dog's water intake, appetite, urination frequency, energy level, and any new symptoms so you can share objective data at monitoring appointments. Provide a balanced, moderate-fat diet and work with your vet on a gentle, consistent exercise routine to help maintain muscle mass without overexerting your dog, since cortisol excess contributes to muscle wasting and fatigue. Protect your dog's fragile skin by using a padded bed, avoiding rough grooming tools, and monitoring for new skin infections or slow-healing wounds that need veterinary attention. Finally, never miss scheduled blood work and ACTH stimulation monitoring appointments, as dosage adjustments are a normal and expected part of long-term Cushing's management and catching changes early prevents dangerous cortisol crashes.

Frequently Asked Questions
What is the life expectancy of a dog diagnosed with Cushing's disease?
With appropriate treatment and regular monitoring, many dogs with pituitary-dependent Cushing's disease live two to three years or more after diagnosis, and some live significantly longer with excellent quality of life. Prognosis depends on the type of Cushing's, the dog's age, and whether secondary complications such as diabetes or blood clots have developed. Adrenal tumors that are benign and surgically removed can carry an even better long-term prognosis.
How is Cushing's disease different from Addison's disease in dogs?
Cushing's disease and Addison's disease are essentially opposite endocrine disorders — Cushing's involves too much cortisol, while Addison's disease (hypoadrenocorticism) involves too little cortisol and often too little aldosterone. Addison's typically presents with vomiting, diarrhea, weakness, and potentially life-threatening electrolyte imbalances, whereas Cushing's develops more slowly with increased thirst, urination, and appetite. Ironically, over-treatment of Cushing's disease with trilostane or mitotane can trigger an iatrogenic Addisonian crisis.
Can Cushing's disease in dogs be cured without surgery?
Medical management with trilostane or mitotane controls Cushing's disease effectively but does not cure it — the underlying pituitary or adrenal tumor remains, and medication must be continued for the rest of the dog's life. Surgical removal of an adrenal tumor (adrenalectomy) can be curative in adrenal-dependent cases, though not all tumors are operable. Transsphenoidal surgery to remove pituitary tumors is performed at a small number of veterinary specialty centers but is not widely available.
How often does a dog on trilostane need blood work and monitoring?
After starting trilostane, most veterinarians perform an ACTH stimulation test at 10 to 14 days, again at 30 days, then at 90 days, and every three to six months thereafter once the dog is stable on an appropriate dose. Additional testing is needed any time the dose is changed or the dog shows concerning symptoms such as lethargy, vomiting, or loss of appetite. Consistent monitoring is the cornerstone of safe, effective Cushing's management.
Are certain dog breeds more prone to developing Cushing's disease?
Yes, several breeds have a higher incidence of Cushing's disease, including Poodles, Dachshunds, Boston Terriers, Boxers, Beagles, and German Shepherds, though any breed can be affected. The condition is most commonly diagnosed in dogs over six years of age, and some studies suggest a slight predisposition in female dogs. Breed predisposition is thought to relate to genetic factors influencing pituitary gland function and adrenal sensitivity.
References
- Behrend, E.N. et al. (2013). "Diagnosis of Spontaneous Canine Hyperadrenocorticism: 2012 ACVIM Consensus Statement." Journal of Veterinary Internal Medicine, 27(6), 1292-1304.
- Merck Veterinary Manual — "Hyperadrenocorticism in Dogs." Available at: merckvetmanual.com.
- Cornell University College of Veterinary Medicine — "Cushing's Syndrome in Dogs." Available at: vet.cornell.edu.
- VCA Animal Hospitals — "Cushing's Disease in Dogs." Available at: vcahospitals.com.
