Quick Answer
An in-depth guide to feline asthma and bronchitis covering pathophysiology, diagnostic imaging, bronchodilator and corticosteroid therapy, inhaler use, and long-term management strategies.
Key Takeaways
- ✓Feline asthma affects 1–5% of cats and is caused by allergic inflammation of the lower airways, similar to human asthma.
- ✓Inhaled fluticasone (Flovent) via an AeroKat spacer is the preferred long-term treatment, delivering steroids directly to the airways with minimal systemic side effects.
- ✓Bronchodilators like albuterol provide acute relief but must always be paired with anti-inflammatory therapy.
- ✓Environmental modification — eliminating smoke, dust, and aerosol irritants — significantly reduces episode frequency.
- ✓A cat in open-mouth breathing or respiratory distress needs immediate emergency veterinary care.
Understanding Feline Asthma
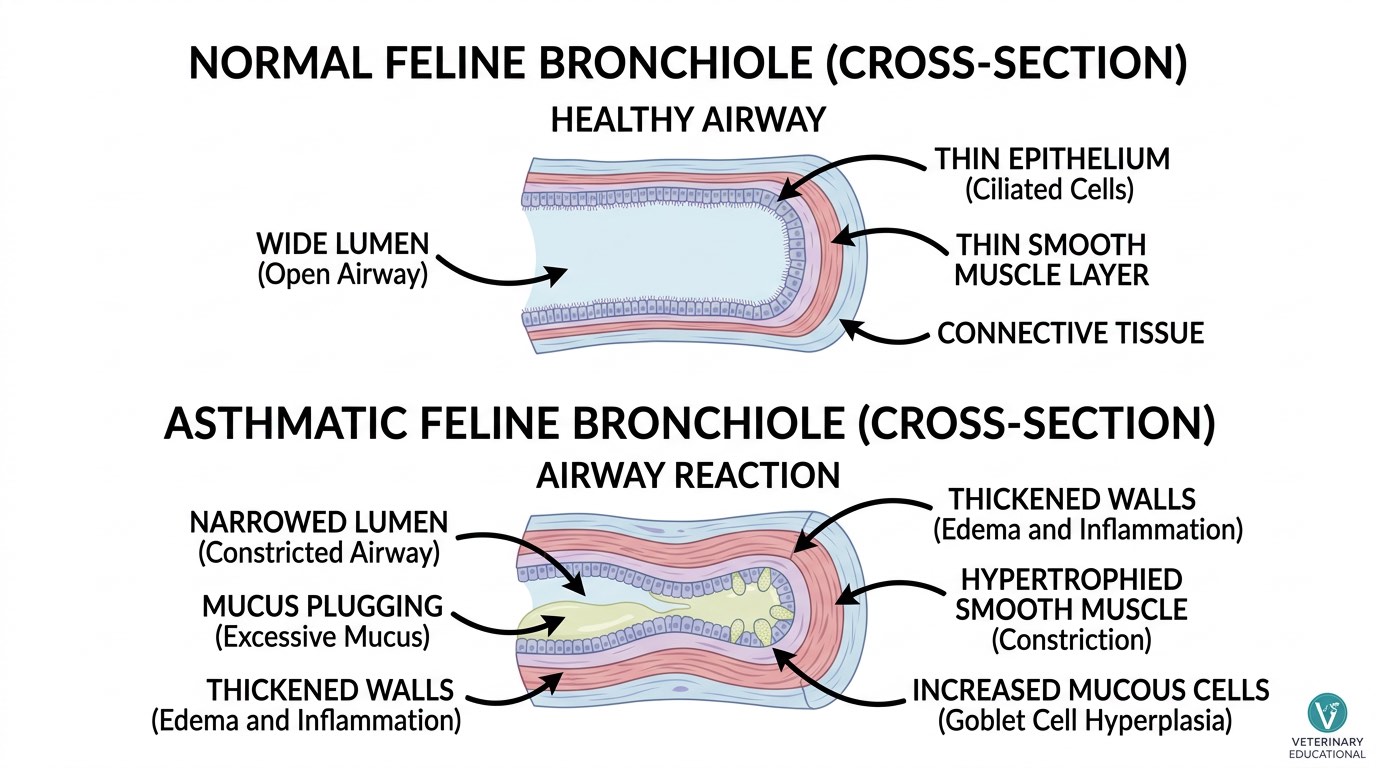
Feline asthma is a chronic inflammatory condition of the lower airways that affects an estimated 1 to 5 percent of all cats. It is characterized by reversible bronchoconstriction, airway inflammation, and excessive mucus production — pathological changes remarkably similar to human asthma. When a susceptible cat inhales an allergen or irritant, the immune system triggers an exaggerated inflammatory response in the bronchial walls, causing smooth muscle spasm, swelling of the airway lining, and accumulation of mucus that narrows the air passages.
The hallmark clinical sign is episodic coughing and wheezing. Owners often describe a characteristic posture: the cat crouches low with its neck extended and produces a dry, hacking cough that can be mistaken for trying to bring up a hairball. In severe episodes, cats may exhibit open-mouth breathing, cyanosis (bluish gums), and marked respiratory distress — a genuine emergency requiring immediate veterinary intervention.
Feline bronchitis is a closely related condition involving chronic inflammation of the bronchi without the classic reversible bronchoconstriction. In practice, the two conditions frequently overlap, and many clinicians use the umbrella term "chronic lower airway disease" when discussing both entities together.
Causes & Common Triggers
Feline asthma is fundamentally an allergic and inflammatory condition. The underlying predisposition is likely genetic, but environmental triggers play a critical role in initiating and perpetuating airway inflammation.
Common Environmental Triggers
Identified triggers vary between individual cats, but the most frequently implicated include:
- Cigarette smoke — one of the strongest documented risk factors for feline respiratory disease
- Dust and dusty cat litter — clay-based clumping litters are particularly problematic
- Household aerosols — air fresheners, cleaning sprays, and perfumes
- Pollen and mold spores — seasonal exacerbations are well documented
- Scented candles and incense — particulate irritants that concentrate in indoor air
- Dust mites — a perennial allergen found in bedding, carpets, and upholstered furniture
The Role of Eosinophilic Inflammation
The hallmark pathological finding in feline asthma is eosinophilic infiltration of the bronchial walls. Eosinophils are white blood cells associated with allergic responses. When activated in the airways, they release inflammatory mediators that damage the epithelial lining, stimulate mucus-producing cells, and promote smooth muscle hypertrophy — all changes that progressively worsen airway function over time.
This is why long-term anti-inflammatory therapy is the cornerstone of treatment. Without ongoing inflammation control, repeated episodes lead to airway remodeling — permanent structural changes that make the airways increasingly resistant to treatment.

Diagnosing Feline Asthma
There is no single definitive test for feline asthma. Diagnosis is based on a combination of clinical signs, imaging findings, and exclusion of other causes of coughing and respiratory distress in cats.
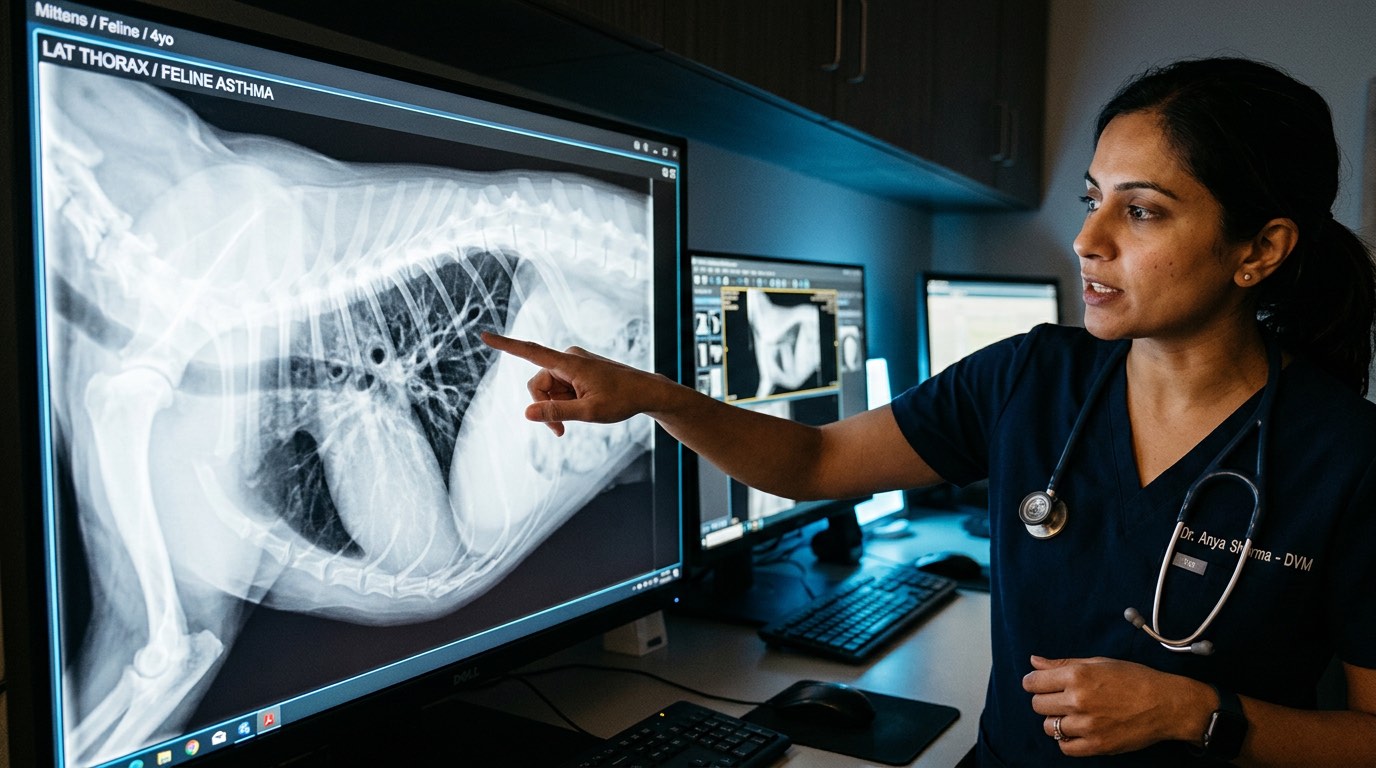
Thoracic Radiography
Chest X-rays are the first-line diagnostic tool. Classic radiographic findings in asthmatic cats include a diffuse bronchial pattern (thickened bronchial walls visible as "donuts" on end-on views and "tramlines" on longitudinal views), hyperinflation of the lungs due to air trapping, and in some cases lung lobe collapse from mucus plugging. However, radiographs can appear normal in mildly affected cats, so a normal X-ray does not rule out the disease.
Bronchoalveolar Lavage (BAL)
BAL involves instilling sterile saline into the airways through an endotracheal tube under general anesthesia, then retrieving the fluid for cytological analysis. Findings of eosinophilic inflammation (greater than 17 percent eosinophils) strongly support a diagnosis of asthma. BAL also allows culture to rule out bacterial or Mycoplasma infections that can mimic or complicate asthma.
Ruling Out Differential Diagnoses
Several conditions produce similar signs and must be considered:
- Heartworm-associated respiratory disease (HARD) — heartworm testing is essential, especially in endemic areas
- Lungworms — fecal Baermann testing or BAL examination can identify parasitic larvae
- Cardiac disease — echocardiography differentiates cardiac from respiratory causes of dyspnea
- Pulmonary neoplasia — thoracic imaging and potentially CT scanning to evaluate masses
Advanced Imaging
CT scanning provides superior detail of the airways and lung parenchyma compared to radiography. It is increasingly used in referral settings to evaluate the extent of airway remodeling and to identify subtle changes not visible on standard X-rays.
Treatment & Medications
The goals of feline asthma therapy are to reduce airway inflammation, relieve bronchoconstriction during acute episodes, and minimize exposure to environmental triggers. Most cats require lifelong management.
Corticosteroids — The Anti-Inflammatory Foundation
Corticosteroids are the mainstay of asthma treatment because they directly target the underlying eosinophilic inflammation. They can be administered in three forms:
Oral prednisolone is commonly used for initial stabilization and in cats whose owners cannot administer inhaled medication. Typical starting doses are 1–2 mg/kg once daily, gradually tapered to the lowest effective dose. Long-term systemic steroid use carries risks including diabetes mellitus, urinary tract infections, and immunosuppression.
Inhaled corticosteroids — specifically fluticasone propionate (Flovent) delivered through a feline-specific spacer chamber such as the AeroKat — represent the preferred long-term approach. Inhaled steroids deliver medication directly to the airways at much lower systemic doses, dramatically reducing the risk of side effects. Most cats can be trained to accept the spacer with patient, gradual conditioning.
Injectable long-acting steroids (methylprednisolone acetate / Depo-Medrol) provide convenient dosing but carry the highest risk of systemic side effects and are generally reserved for cats that cannot receive oral or inhaled medication.
Bronchodilators — Acute Relief
Bronchodilators relax the smooth muscle surrounding the airways and provide rapid relief during acute bronchoconstriction. Albuterol (salbutamol) delivered via metered-dose inhaler through the AeroKat spacer is the preferred rescue medication. Terbutaline can be given as a subcutaneous injection in emergency settings for cats in severe respiratory distress.
Bronchodilators alone do not address the underlying inflammation and should never be used as sole therapy — doing so can actually worsen long-term outcomes by masking disease progression.
Emergency Management
Cats presenting in acute respiratory distress require oxygen supplementation, injectable bronchodilators (terbutaline), and fast-acting corticosteroids. Minimal handling is critical, as stress can worsen respiratory compromise in these fragile patients.

Living with a Cat with Asthma
Successful long-term management of feline asthma requires a combination of medical therapy and environmental control. With consistent treatment, most asthmatic cats can live comfortable, active lives with normal or near-normal life expectancy.
Environmental Modifications
Reducing allergen and irritant exposure is a critical component of management:
- Switch to low-dust, unscented cat litter (paper-based or crystal litters are often best)
- Eliminate smoking indoors — this single change can dramatically improve respiratory health
- Use unscented, pet-safe cleaning products
- Run HEPA air purifiers in rooms where the cat spends the most time
- Wash bedding regularly in hot water to reduce dust mite populations
- Avoid air fresheners, scented candles, and heavily fragranced products
Monitoring at Home
Owners should learn to monitor their cat's resting respiratory rate (RRR) — the number of breaths per minute while sleeping. A normal cat takes 15–30 breaths per minute at rest. A persistent resting rate above 40 breaths per minute suggests worsening disease and warrants veterinary evaluation. Smartphone apps are available to help track RRR over time.
Keeping a log of coughing episodes — frequency, duration, time of day, and potential triggers — helps veterinarians adjust therapy more precisely.
Prognosis
The majority of cats with well-managed asthma have an excellent long-term prognosis. Cats that develop severe airway remodeling or those with frequent, poorly controlled crises may have a more guarded outlook. The transition from oral steroids to inhaled therapy is strongly encouraged whenever possible to minimize cumulative steroid side effects over a cat's lifetime. Regular veterinary rechecks — typically every 6–12 months for stable patients — allow treatment adjustments before clinical deterioration occurs.

Frequently Asked Questions
How can I tell if my cat has asthma or just hairballs?
Asthmatic coughing involves a characteristic crouched posture with extended neck and produces a dry, hacking sound without bringing up a hairball. Hairball retching typically involves abdominal heaving and produces a tubular mass of hair. If your cat frequently coughs without producing anything, a veterinary evaluation with chest X-rays is recommended.
Can cats use human asthma inhalers?
Cats use the same metered-dose inhaler medications as humans (fluticasone, albuterol), but they require a feline-specific spacer chamber like the AeroKat because they cannot coordinate inhalation with actuation. The spacer holds the aerosolized medication in a chamber so the cat breathes it in naturally over several breaths.
Is feline asthma curable?
Feline asthma is a chronic condition that is managed rather than cured. With appropriate anti-inflammatory therapy and environmental modifications, most cats achieve excellent symptom control and live normal lifespans. Some cats may have periods of remission but remain at risk for future episodes.
How much does feline asthma treatment cost?
Initial diagnostics (X-rays, bloodwork) typically range from $300–$600. An AeroKat spacer costs approximately $50–$80, and inhaler medications (fluticasone, albuterol) cost $30–$80 per canister, lasting 1–3 months depending on dosing frequency. Ongoing costs are generally manageable once the initial workup is complete.
Can indoor air quality affect my cat's asthma?
Absolutely. Indoor air quality is one of the most important controllable factors. Cigarette smoke, scented candles, aerosol sprays, and dusty cat litter are among the most common triggers. Using HEPA air purifiers, switching to low-dust litter, and avoiding airborne irritants can significantly reduce asthma episodes.
References
- Trzil JE. Feline Asthma: Diagnostic and Treatment Update. Veterinary Clinics of North America: Small Animal Practice. 2020;50(2):375-391.
- Reinero CR. Advances in the understanding of pathogenesis, and diagnostics and therapeutics for feline allergic asthma. The Veterinary Journal. 2011;190(1):28-33.
- Venema CM, Patterson CC. Feline asthma: what's new and where might clinical practice be heading? Journal of Feline Medicine and Surgery. 2010;12(9):681-692.
