Quick Answer
Cancer is the leading cause of death in dogs over age 10, affecting nearly one in three dogs at some point in their lives. This comprehensive guide covers the most common types of canine cancer, how to recognize early warning signs, the role of staging and biopsy, and the spectrum of treatment options available — from surgery to immunotherapy.
Key Takeaways
- ✓Cancer affects nearly 1 in 3 dogs; it is the leading cause of death in dogs over age 10
- ✓Lymphoma, mast cell tumors, osteosarcoma, and hemangiosarcoma are among the most common types
- ✓Early detection improves outcomes — any new or growing lump should be aspirated, not watched
- ✓Dogs generally tolerate chemotherapy well, with much less severe side effects than in humans
- ✓A veterinary oncologist consultation provides complete options; it does not obligate aggressive treatment
How Common Is Cancer in Dogs?
Cancer is not rare in dogs — it is the single leading cause of disease-related death in dogs over age 10, accounting for approximately 50% of deaths in that age group. Roughly one in three dogs will develop cancer at some point in their lives, a rate comparable to humans.
Why Dogs Get Cancer
Cancer arises when normal cells undergo genetic mutations that cause uncontrolled proliferation. In dogs, the same fundamental biology applies: damaged DNA, environmental exposures, inherited predispositions, chronic inflammation, and immune dysregulation all contribute.
Certain Breeds Are at Outsized Risk
Unlike in humans where cancer risk is broadly distributed, certain dog breeds carry dramatically elevated cancer rates due to genetic bottlenecks and selective breeding:
- Golden Retrievers: Approximately 60% of Golden Retrievers die of cancer — the highest rate of any breed studied. A large-scale Morris Animal Foundation study (the Golden Retriever Lifetime Study) is actively investigating why.
- Bernese Mountain Dogs: High rates of histiocytic sarcoma, a particularly aggressive cancer
- Boxers: Elevated rates of mast cell tumors and brain tumors
- Rottweilers: High rates of osteosarcoma and lymphoma
- Scottish Terriers: 20× the normal risk of transitional cell carcinoma (bladder cancer)
- Flat-Coated Retrievers: High lifetime cancer risk, similar to Golden Retrievers
Age and Cancer Risk
Cancer becomes increasingly common after age 7. Large and giant breeds, which age faster, tend to develop cancer at younger ages than small breeds. A 7-year-old Great Dane is physiologically older than a 7-year-old Chihuahua.

The 7 Most Common Canine Cancers
1. Lymphoma (Lymphosarcoma)
Lymphoma is one of the most common canine cancers, affecting lymphocytes (immune cells). It most often presents as painless, rapidly enlarging lymph nodes — owners typically notice lumps in the neck, behind the knees, or in the armpits. Multicentric lymphoma (affecting multiple lymph node sites) is the most frequent form. Chemotherapy with the CHOP protocol achieves remission in 80–90% of dogs, with a median survival of 12–14 months. Some dogs live 2+ years.
2. Mast Cell Tumors (MCT)
Mast cell tumors are the most common skin tumor in dogs. They range from benign-behaving low-grade tumors to highly aggressive high-grade tumors that spread rapidly to internal organs. Boxers, Bulldogs, and Labrador Retrievers are among the most frequently affected breeds. Grade and biological behavior are determined by histopathology. Surgical excision with adequate margins is curative for low-grade tumors; high-grade MCT requires surgery plus chemotherapy.
3. Osteosarcoma (Bone Cancer)
Osteosarcoma is the most common bone tumor in dogs and predominantly affects large and giant breeds — Rottweilers, Irish Wolfhounds, Great Danes, and Saint Bernards are at particular risk. It typically affects the long bones near joints (distal radius, proximal humerus, distal femur). Lameness and progressive bone pain are the presenting signs; x-ray shows characteristic bone lysis and "sunburst" periosteal reaction. Without treatment, median survival is 1–4 months. Limb amputation followed by chemotherapy extends median survival to 10–12 months; limb-sparing surgeries are possible in some cases.
4. Hemangiosarcoma
Hemangiosarcoma arises from blood vessel endothelial cells and most commonly affects the spleen, heart (right atrium), and liver. It is particularly prevalent in German Shepherds and Golden Retrievers. Splenic hemangiosarcoma often causes no signs until the tumor ruptures, producing sudden internal hemorrhage and collapse — owners describe a dog who was "fine yesterday." Surgery to remove the spleen may save the dog from acute hemorrhage, but median survival with surgery alone is only 1–2 months. With post-surgical chemotherapy, median survival extends to 4–6 months.
5. Transitional Cell Carcinoma (Bladder Cancer)
TCC originates in the lining of the urinary bladder, most commonly at the trigone (the outlet of the bladder — the worst possible location for surgical removal). Signs include frequent urination, blood in urine, and straining. Scottish Terriers, Beagles, Shetland Sheepdogs, and West Highland White Terriers are at elevated risk. A non-invasive urine test (CADET BRAF) can detect TCC in high-risk dogs. Medical management with piroxicam (an NSAID with anti-tumor properties) and chemotherapy can achieve disease control in many cases.
6. Histiocytic Sarcoma
This aggressive cancer of histiocytes (immune cells) is strongly associated with Bernese Mountain Dogs, Flat-Coated Retrievers, and Rottweilers. It often spreads rapidly to the spleen, lungs, and brain. Median survival is short (weeks to a few months) even with chemotherapy, though CCNU (lomustine) is the standard of care.
7. Soft Tissue Sarcomas (STS)
A broad category of tumors arising from connective tissue (fibrosarcoma, peripheral nerve sheath tumor, etc.). They typically present as firm, subcutaneous masses. Surgical excision with wide margins is the primary treatment; local recurrence is common if margins are not adequate. They tend to recur locally rather than spread early to distant sites.
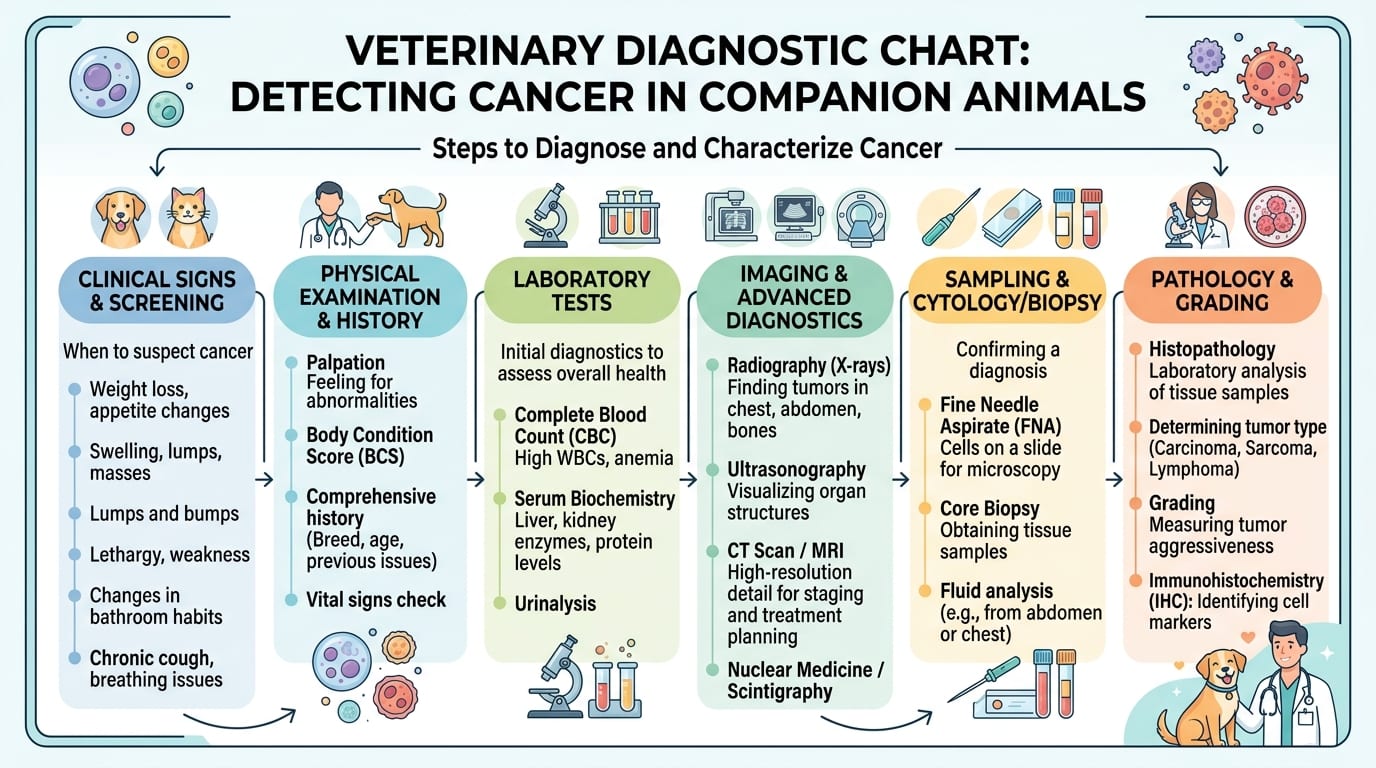
Early Warning Signs of Cancer in Dogs
The Veterinary Cancer Society and many oncology specialists advocate using the acronym CAUTION to remember the key signs of potential cancer in pets:
- Change in bowel or bladder habits
- A sore that does not heal
- Unusual bleeding or discharge
- Tumor or lump in or under the skin
- Indigestion or difficulty swallowing
- Obvious weight loss
- Not interested in exercise; loss of energy
Other Signs to Watch For
- Lameness or limping that doesn't improve (especially in large breeds — suspect bone cancer)
- Persistent coughing or difficulty breathing
- Abdominal swelling
- Pale gums (internal bleeding from splenic or hepatic tumors)
- Sudden collapse
When to See a Veterinarian
Any lump that is new, growing, or changing in character should be evaluated. Many lumps in dogs are benign (lipomas, sebaceous cysts) but the only way to know is by sampling the cells — a simple needle aspirate is often sufficient for an initial answer. Do not wait and watch a lump for months. The cost of an aspirate ($50–$150) is a small investment for important information.
Similarly, any unexplained lameness in a large breed dog over age 5 that persists beyond 1–2 weeks should include x-rays to evaluate for bone cancer.

Diagnosis, Staging & What to Expect
Step 1: Fine Needle Aspirate (FNA)
For superficial masses, an FNA — inserting a needle into the mass and withdrawing cells for microscopic examination — is the quickest and least invasive first step. It can often differentiate between mast cell tumors, lipomas, and other tumors, though it cannot provide the full architectural information of a biopsy.
Step 2: Biopsy and Histopathology
A tissue biopsy provides definitive diagnosis, tumor grade, and margin assessment (after excision). Grading tells the oncologist how aggressively the tumor is likely to behave and guides treatment decisions.
Step 3: Staging
Staging determines whether the cancer has spread beyond the primary site. Staging may include:
- Regional lymph node aspirates or biopsies
- Chest x-rays (3 views) to check for pulmonary metastasis
- Abdominal ultrasound to evaluate abdominal organs and lymph nodes
- CT scan (increasingly standard of care, especially for solid tumors pre-surgery)
- Bone marrow aspirate (for lymphoma staging)
- Blood tests including CBC, chemistry panel, and urinalysis
Step 4: Referral to a Veterinary Oncologist
Board-certified veterinary oncologists (DACVIM-Oncology) specialize in cancer treatment planning. Many veterinary schools and specialty hospitals have dedicated oncology services. Consulting an oncologist does not obligate you to pursue aggressive treatment — it ensures you have complete information about your options.

Treatment Options in Modern Veterinary Oncology
Modern veterinary oncology has access to many of the same treatment modalities as human oncology, though with adaptations for canine biology.
Surgery
Surgical excision remains the primary treatment for most solid tumors. The goal is to remove the tumor with adequate "clean margins" — a rim of normal tissue surrounding the tumor. The required margin width varies by tumor type. Surgery can be curative for many low-grade soft tissue sarcomas and mast cell tumors caught early.
Chemotherapy
Dogs generally tolerate chemotherapy significantly better than humans. This is because veterinary oncologists dose to control disease while maintaining quality of life — they typically do not push to the maximum tolerated dose the way human oncologists sometimes do. Hair loss is rare in dogs (except in curly-coated breeds). Most dogs maintain normal activity levels during treatment. Common protocols include CHOP (cyclophosphamide, doxorubicin, vincristine, prednisone) for lymphoma; carboplatin for osteosarcoma; and lomustine for mast cell tumors and histiocytic sarcoma.
Radiation Therapy
Radiation is used for tumors that cannot be fully surgically excised (particularly brain tumors, nasal tumors, and residual disease post-surgery). Stereotactic radiosurgery (SRS) — similar to CyberKnife in humans — delivers precisely targeted radiation to tumors in as few as 1–3 sessions. It is transforming the treatment of brain tumors and other previously difficult-to-treat cancers.
Targeted Therapy and Immunotherapy
Toceranib phosphate (Palladia) is an oral tyrosine kinase inhibitor approved for mast cell tumors — one of the first targeted cancer drugs developed specifically for dogs. Immunotherapy (checkpoint inhibitors, cancer vaccines) is an active area of veterinary oncology research. Early results in canine melanoma and osteosarcoma are promising.
Palliative and Supportive Care
When curative intent is not feasible or not chosen, palliative care focuses on controlling pain, maintaining appetite, and preserving quality of life. NSAIDs (particularly piroxicam and meloxicam) have anti-tumor properties and are a cornerstone of palliative protocols for many cancers. Palliative care can extend good-quality survival time in many patients.

Frequently Asked Questions
Is cancer painful for dogs?
Cancer-related pain varies by tumor type and location. Bone cancer (osteosarcoma) is notoriously painful. Internal tumors may cause discomfort without obvious pain signals. Dogs often hide pain instinctively, so behavioral changes — reduced activity, reluctance to jump, altered sleeping position, or changes in appetite — may be the only signs. Pain management is a central part of both curative and palliative cancer care.
How do I know if my dog's lump is cancer?
You cannot determine whether a lump is cancerous by looking at or feeling it — size, location, texture, and growth rate are poor predictors of malignancy. A fine needle aspirate (FNA) performed by your veterinarian is the only way to get a meaningful initial answer. Some tumors require a formal biopsy for definitive typing and grading. Do not delay evaluation of new lumps.
What is the average survival time for a dog with cancer?
Survival time varies enormously by cancer type, grade, and stage at diagnosis. Early-stage mast cell tumors removed surgically can be cured. Lymphoma in remission averages 12–14 months with treatment. Osteosarcoma averages 10–12 months with amputation and chemotherapy. Hemangiosarcoma averages 4–6 months. These are averages — individual dogs may do much better or worse. Consulting a veterinary oncologist for your specific situation gives the most meaningful prognosis.
Should I pursue chemotherapy for my dog?
This is a deeply personal decision that depends on the specific cancer, your dog's overall health, the expected benefit, and your family's values and resources. Veterinary chemotherapy is designed to maintain quality of life — most dogs are not nauseated or incapacitated during treatment. A candid conversation with a veterinary oncologist about realistic expectations, costs, and quality of life during treatment will help you make the right decision for your dog.
References
- Withrow SJ, Vail DM, Page R. Withrow & MacEwen's Small Animal Clinical Oncology. 5th ed. Saunders Elsevier, 2013.
- Paoloni M, Khanna C. "Translation of new cancer treatments from pet dogs to humans." Nat Rev Cancer. 2008;8(2):147-156.
- Dobson JM. "Breed-predispositions to cancer in pedigree dogs." ISRN Vet Sci. 2013.
