Quick Answer
An in-depth guide to canine osteoarthritis — the most common cause of chronic pain in dogs. Covers how joints degenerate, the subtle early signs owners miss, diagnosis with orthopedic exam and X-rays, and the full range of treatments from NSAIDs and Librela to physical therapy, laser treatment, acupuncture, and joint supplements.
Key Takeaways
- ✓Osteoarthritis affects an estimated 80% of dogs over 8 years old — it is dramatically underdiagnosed because dogs hide pain
- ✓Early signs include hesitation before jumping, stiffness after rest, reduced activity, and behavioral changes — not just obvious limping
- ✓Librela (monthly monoclonal antibody injection) is a major advance — it targets a different pain pathway than NSAIDs and is highly effective
- ✓Multimodal management combining NSAIDs or Librela with rehabilitation, laser therapy, omega-3s, and environmental modifications gives the best outcomes
- ✓Weight control is the highest-impact lifestyle intervention — even modest weight loss significantly reduces lameness in overweight arthritic dogs
Understanding Canine Osteoarthritis
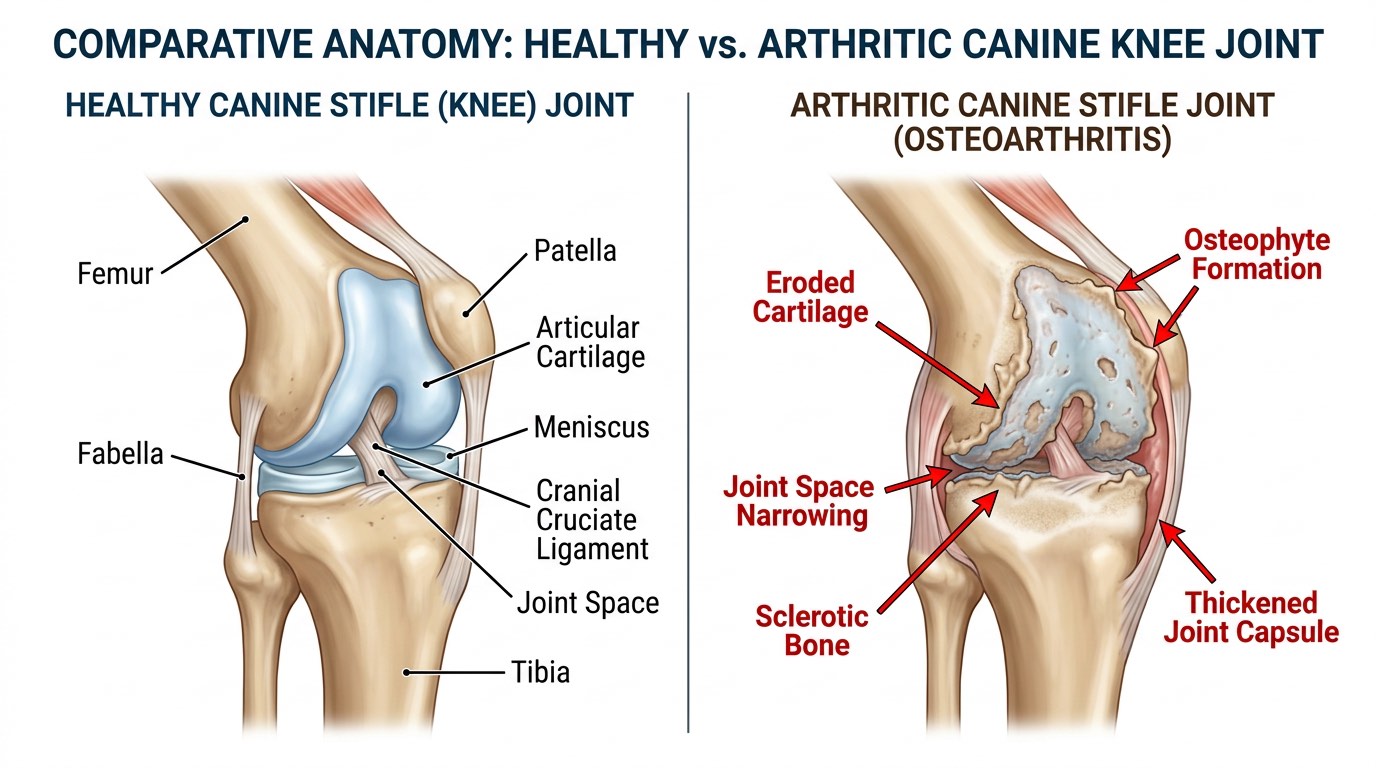
Osteoarthritis (OA) — also called degenerative joint disease (DJD) — is a progressive condition in which the protective cartilage lining the ends of bones within a joint gradually breaks down. As cartilage thins and erodes, the underlying bone is exposed, leading to bone-on-bone friction, inflammation of the joint lining (synovitis), the formation of bony outgrowths called osteophytes, and eventually significant structural remodeling of the joint. The result is a joint that is painful, stiff, and has reduced range of motion.
Osteoarthritis affects an estimated 20% of all adult dogs and 80% of dogs over 8 years old — making it one of the most prevalent chronic conditions in veterinary medicine. Despite these numbers, it is dramatically underdiagnosed: dogs are stoic by nature and express pain differently than humans. Slowing down is often attributed to "just getting old" when in reality the dog is living with significant chronic pain that responds well to treatment.
OA can be primary (idiopathic, occurring without an identifiable cause in older dogs) or secondary (arising from underlying joint abnormalities such as hip dysplasia, elbow dysplasia, cruciate ligament disease, or previous joint injury). Secondary OA is more common in younger dogs and large breeds. Both forms follow the same progressive course and respond to the same management strategies, though addressing the underlying cause in secondary OA is an important additional step.
The Subtle Signs of Arthritis Dogs Hide
Dogs do not vocalize pain the way humans do. They adapt their movement to avoid discomfort, and owners often mistake these adaptations for normal aging. Knowing what to look for makes early identification possible — and early intervention makes a meaningful difference in long-term outcomes.
The earliest signs of OA are often behavioral and subtle: hesitating before jumping into the car or onto furniture, choosing not to climb stairs they once navigated freely, taking longer to rise from rest, or appearing stiff for the first few minutes of a walk before "warming up." Some dogs begin sleeping more, playing less, or showing uncharacteristic irritability when touched in certain areas. These early signs are easy to miss precisely because they develop gradually.
As OA progresses, owners notice more obvious lameness — favoring one leg, a shortened stride, or an asymmetric gait. Muscle atrophy in the affected limb(s) occurs because the dog uses those muscles less. In advanced disease, the dog may cry or flinch when the affected joint is manipulated, have visible joint swelling, and show significant reluctance to exercise. The Five-Minute Orthopaedic Observation — watching your dog rise from rest, walk in a straight line, trot, and go up/down stairs — is a useful home assessment to discuss at vet visits.

Diagnosis: Orthopedic Exam, X-rays, and Scoring
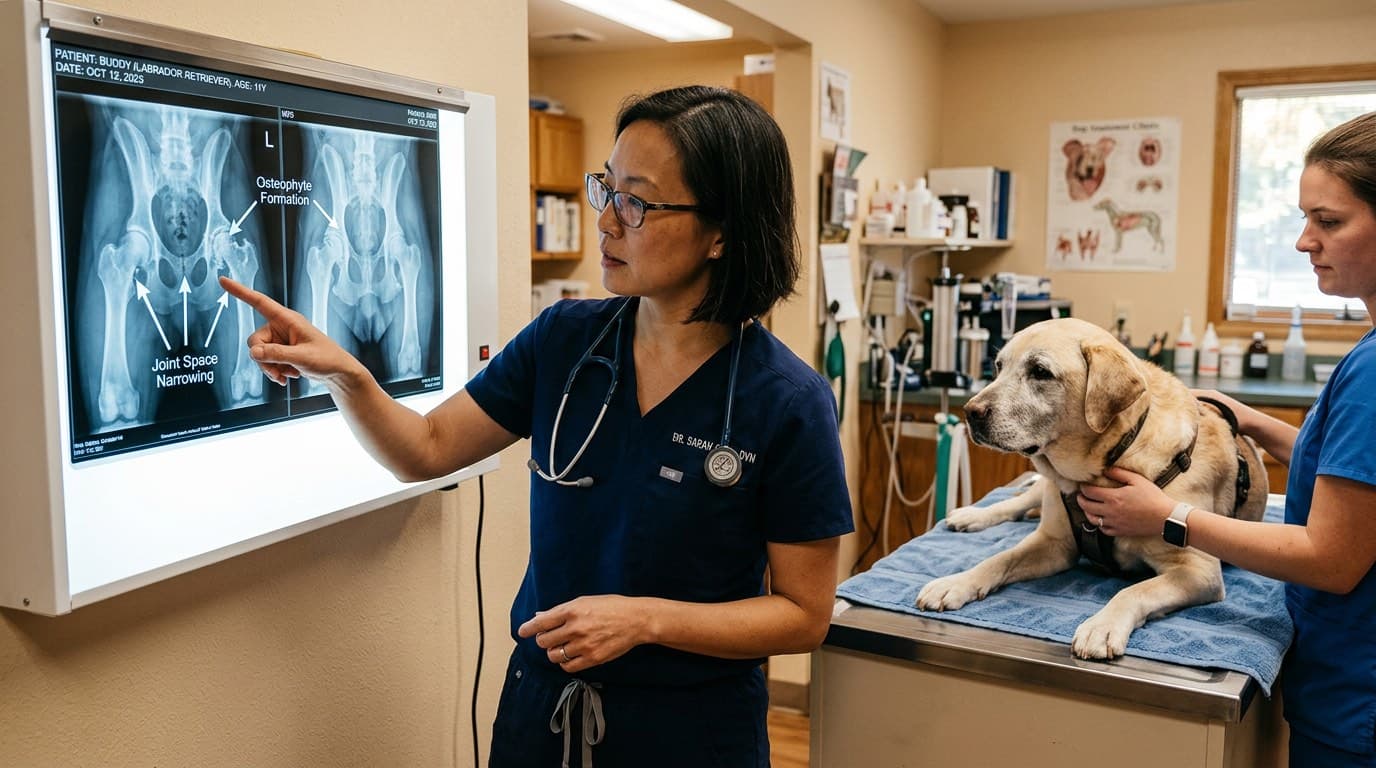
Diagnosis begins with a thorough orthopedic examination in which the veterinarian evaluates gait, palpates each joint for pain, swelling, and crepitus (a grating sensation), and assesses range of motion in all major joints. Dogs should ideally be assessed after a period of rest AND after moderate activity, since some OA patients are stiffer after rest and others worsen with activity.
Radiography (X-rays) is the primary imaging modality for confirming OA. Classic radiographic findings include joint space narrowing, osteophyte formation, subchondral bone sclerosis, and soft tissue swelling. It is important to note that radiographic severity does not always correlate with clinical pain — some dogs with dramatic X-ray changes are relatively comfortable, while others with minimal radiographic changes experience severe pain. CT imaging provides more detailed bone evaluation, particularly for complex joints like the elbow, and MRI is superior for evaluating soft tissue and cartilage.
Pain scoring systems such as the Canine Brief Pain Inventory (CBPI) and the Helsinki Chronic Pain Index allow owners to systematically rate their dog's pain and mobility limitations, providing an objective measure of treatment response over time. Your veterinarian may ask you to complete one of these questionnaires at each visit.
Treatment: NSAIDs, Librela, and Multimodal Approaches
Effective OA management in dogs requires a multimodal approach — no single treatment addresses all aspects of the disease, and combining therapies provides synergistic benefit. The foundation of medical management is non-steroidal anti-inflammatory drugs (NSAIDs) specifically formulated for dogs: carprofen, meloxicam, grapiprant, deracoxib, and others. These reduce joint inflammation and provide meaningful pain relief. Dogs on long-term NSAIDs require baseline bloodwork and periodic monitoring (every 6 months) to check kidney and liver function.
Librela (bedinvetmab) — introduced in recent years — is a monthly monoclonal antibody injection that targets nerve growth factor (NGF), a key mediator of OA pain. It works by a completely different mechanism than NSAIDs, making it an excellent option for dogs that do not tolerate NSAIDs well, dogs that need additional pain control alongside NSAIDs, or as a primary treatment when NSAIDs are contraindicated. Clinical trials showed significant reductions in pain and improvements in mobility in arthritic dogs.
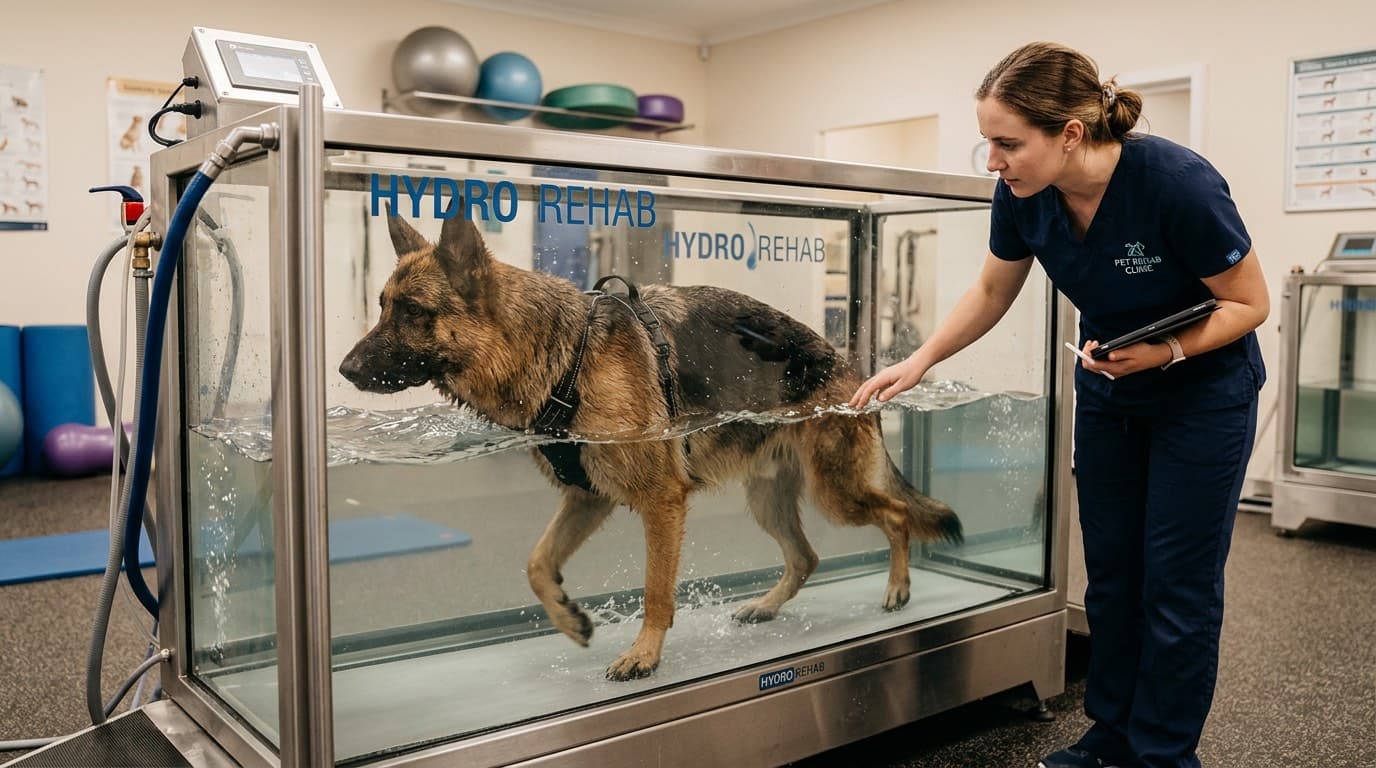
Adjunctive therapies with strong evidence include: veterinary rehabilitation (physical therapy, underwater treadmill hydrotherapy, therapeutic exercises), therapeutic laser (low-level laser therapy reduces inflammation and promotes tissue healing), and acupuncture. Joint supplements containing glucosamine and chondroitin have mild evidence; omega-3 fatty acids from fish oil have more robust evidence for anti-inflammatory benefits. Adequan (polysulfated glycosaminoglycan) injections help maintain joint fluid viscosity and have disease-modifying properties in early OA.
Home Care: Exercise, Environment, and Weight Control
Weight management is arguably the single most impactful intervention for arthritic dogs that are overweight. Each additional kilogram of body weight adds roughly four kilograms of force to joints with every step. Studies consistently show that weight loss alone significantly reduces lameness scores in overweight OA dogs. If your arthritic dog is even moderately overweight, a structured weight loss plan under veterinary guidance should be a top priority.
Exercise remains important for arthritic dogs — but the type, duration, and intensity must be adjusted. Short, frequent, gentle walks on soft surfaces (grass, dirt) are preferable to long hikes on hard pavement. Controlled leash walking is better than off-leash running where the dog may overdo it and pay for it the next day. Avoid activities that require jumping, sudden direction changes, or prolonged stair climbing. Swimming is excellent for OA dogs — it provides cardiovascular and muscular conditioning with near-zero joint loading.
Environmental modifications make a meaningful quality-of-life difference: orthopedic memory foam beds reduce pressure on stiff joints, raised food and water bowls reduce neck and shoulder strain, ramps or pet stairs to furniture and vehicles eliminate the need to jump, non-slip rugs on slippery floors prevent falls and reduce the effort of rising, and baby gates block access to stairs if needed. Warm environments reduce morning stiffness — some owners find a warm (not hot) water bottle wrapped in a towel placed near the sleeping area helpful on cold nights.

Frequently Asked Questions
How do I know if my dog is in pain from arthritis?
Dogs rarely cry or whimper from arthritis pain. Instead, watch for subtle behavioral changes: reluctance to jump or climb stairs, stiffness after rest (especially in the morning), shorter walks, decreased play interest, changes in sleeping position, or irritability when touched. The more of these signs you notice, the more likely chronic pain is involved — a veterinary orthopedic evaluation is warranted.
What is Librela and how is it different from NSAIDs?
Librela (bedinvetmab) is a monthly monoclonal antibody injection that blocks nerve growth factor (NGF), a protein central to arthritis pain signaling. Unlike NSAIDs, which reduce inflammation broadly, Librela targets pain signaling very specifically. It is safe to use alongside other treatments including NSAIDs in many cases, and has been shown to significantly improve mobility and reduce pain in clinical trials. It is a major advance for dogs that cannot tolerate NSAIDs.
Can young dogs get arthritis?
Yes — secondary osteoarthritis can develop in young and middle-aged dogs as a consequence of underlying joint problems like hip dysplasia, elbow dysplasia, or cruciate ligament injury. Arthritis developing from a prior joint injury can begin as early as 1–2 years of age. This is why treating developmental joint diseases promptly and appropriately is so important.
Are joint supplements like glucosamine effective for dog arthritis?
Evidence for glucosamine/chondroitin supplements in dogs is modest and mixed — they are unlikely to cause harm but should not replace proven treatments like NSAIDs or Librela. Omega-3 fatty acids from fish oil have stronger evidence for reducing joint inflammation and are more reliably beneficial. Adequan (polysulfated glycosaminoglycan) injections have better clinical evidence than oral supplements for supporting joint health.
Is it okay to exercise an arthritic dog?
Yes — controlled, low-impact exercise is beneficial and important for arthritic dogs. Short, frequent walks on soft surfaces, swimming, and gentle rehabilitation exercises maintain muscle mass, support joint stability, and improve mood. The key is avoiding high-impact activities (running off-leash, jumping, prolonged stair climbing) and reading your dog's post-exercise response — if they are significantly stiffer the next day, the intensity was too high.
References
- Johnston SA. Osteoarthritis: joint anatomy, physiology, and pathobiology. Vet Clin North Am Small Anim Pract. 1997.
- Enomoto M, et al. Bedinvetmab, a canine anti-NGF monoclonal antibody, in dogs with OA pain. J Vet Pharmacol Ther. 2022.
- Rychel JK. Diagnosis and treatment of osteoarthritis. Top Companion Anim Med. 2010.
- Marshall WG, et al. The effect of weight loss on lameness in obese dogs with OA. Vet Res Commun. 2010.
