Quick Answer
An in-depth guide to feline hyperthyroidism covering thyroid adenoma pathology, clinical signs, T4 testing and diagnosis, and the four major treatment options — methimazole, radioiodine therapy (I-131), thyroidectomy, and iodine-restricted diet — to help cat owners make informed decisions.
Key Takeaways
- ✓Hyperthyroidism is the most common endocrine disease in cats and is almost always caused by a benign thyroid adenoma producing excess thyroid hormones
- ✓Classic signs include weight loss despite increased appetite, hyperactivity, increased thirst and urination, and intermittent vomiting — though some cats present with lethargy and poor appetite instead
- ✓A serum total T4 blood test is the primary diagnostic tool, but additional testing may be needed for early or borderline cases
- ✓Radioiodine therapy (I-131) is the gold standard cure with over 95% success rate, while methimazole provides effective lifelong medical management
- ✓A methimazole trial before permanent treatment is essential because normalizing thyroid levels can unmask hidden chronic kidney disease
What Is Feline Hyperthyroidism?
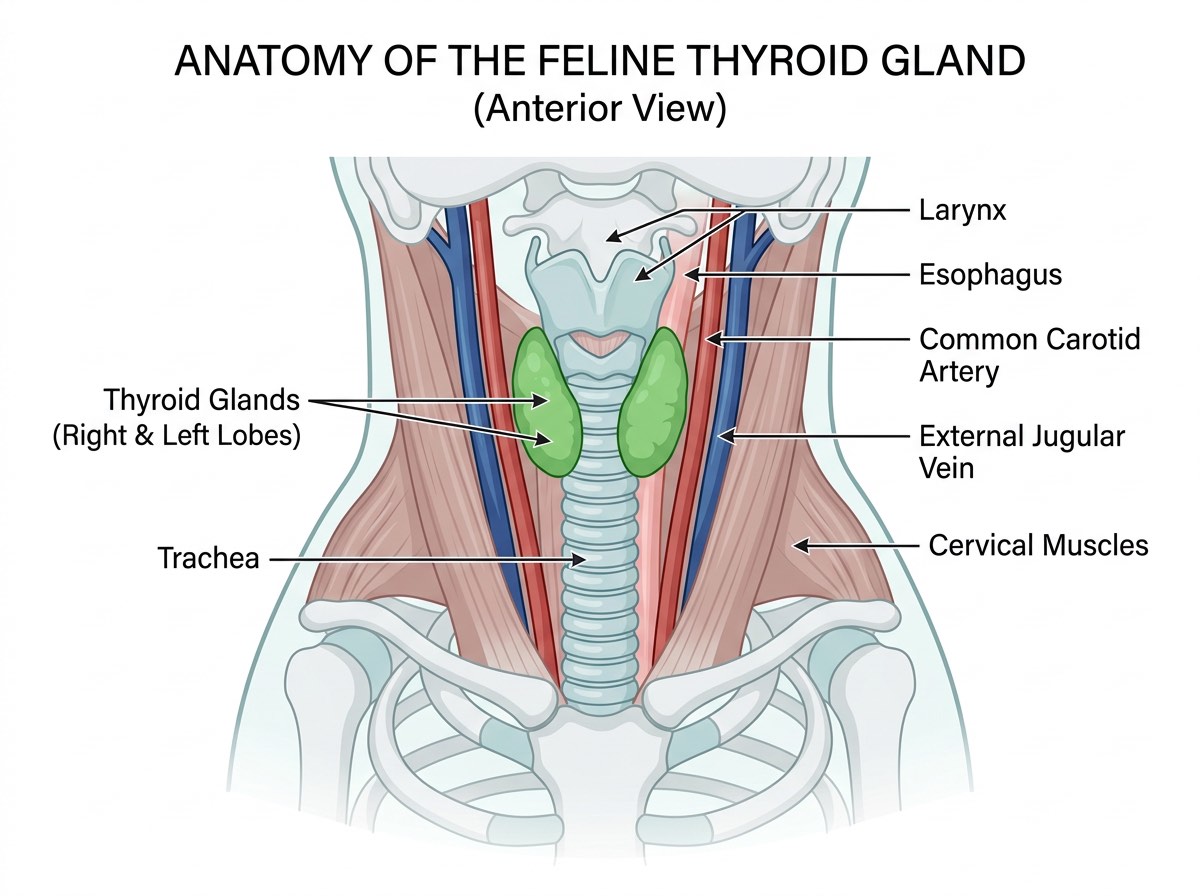
Hyperthyroidism is the most common endocrine disorder in cats, predominantly affecting middle-aged and senior felines over the age of eight. The condition results from the overproduction of thyroid hormones — primarily thyroxine (T4) and triiodothyronine (T3) — by one or both thyroid glands located in the neck. In approximately 97 to 99 percent of cases, the underlying cause is a benign functional thyroid adenoma (adenomatous hyperplasia), while thyroid carcinoma accounts for fewer than two to three percent of cases.
The excess thyroid hormone accelerates the body's metabolic rate, affecting virtually every organ system. Cats with hyperthyroidism typically exhibit a characteristic combination of weight loss despite a ravenous appetite, increased thirst and urination, restlessness, hyperactivity, and intermittent vomiting or diarrhea. Untreated hyperthyroidism places significant strain on the heart, often leading to a secondary condition called thyrotoxic hypertrophic cardiomyopathy — a thickening of the heart muscle walls that can progress to congestive heart failure if left unaddressed.
Since hyperthyroidism was first recognized in cats in 1979, its diagnosis has increased dramatically, though whether this reflects a true increase in prevalence or improved detection remains debated. Environmental factors — including exposure to flame retardants (polybrominated diphenyl ethers), certain canned food linings, and indoor living — have been investigated as potential contributing causes, though no single factor has been definitively established.
Recognizing the Signs
The clinical signs of feline hyperthyroidism develop gradually and may initially be mistaken for normal aging. Weight loss is the most consistent finding, often occurring despite a normal or increased appetite — a combination that should always raise clinical suspicion in a middle-aged or older cat. Many owners describe their cat as seeming "younger" or more energetic than usual, with increased vocalization, restlessness, and nighttime activity. While this hyperactivity may initially seem like a positive change, it reflects a pathologically elevated metabolic rate.
Gastrointestinal signs are common and include intermittent vomiting, increased stool volume, and occasionally diarrhea. Polydipsia (increased water intake) and polyuria (increased urination) occur as the kidneys process a higher volume of blood flow. The cat's coat may become unkempt, greasy, or matted because the accelerated metabolism diverts energy away from normal grooming and coat maintenance. In some cats, particularly those with advanced disease, a palpable thyroid nodule — sometimes called a "thyroid slip" — can be felt by a veterinarian during a physical examination of the neck.
A subset of cats presents with what is termed "apathetic hyperthyroidism," showing lethargy, decreased appetite, and depression rather than the classic hyperactive presentation. This form is less common but important to recognize because it can mimic other serious illnesses and may delay diagnosis. Cardiac complications, including an elevated heart rate (tachycardia), heart murmurs, and gallop rhythms, are present in a significant proportion of hyperthyroid cats and underscore the systemic impact of untreated disease.

How Hyperthyroidism Is Diagnosed
Diagnosis of feline hyperthyroidism typically begins with a thorough physical examination, during which the veterinarian may palpate an enlarged thyroid gland in the neck and assess the heart rate, body condition, and overall demeanor. The confirmatory test is a serum total thyroxine (total T4) level, which is elevated above the normal reference range in the majority of hyperthyroid cats. This blood test is widely available, relatively inexpensive, and highly reliable for straightforward cases.
However, some cats with early-stage or mild hyperthyroidism may have total T4 levels that fall within the upper end of the normal range — a situation referred to as "occult hyperthyroidism." In these cases, the veterinarian may recommend additional testing including a free T4 by equilibrium dialysis, which is more sensitive at detecting mildly elevated thyroid function. Serial monitoring of total T4 over several weeks, or thyroid scintigraphy (a nuclear medicine scan using technetium-99m pertechnetate) at a specialty center, can confirm the diagnosis and identify whether one or both thyroid lobes are affected.
A complete diagnostic workup also includes a complete blood count (CBC), serum biochemistry panel, and urinalysis to evaluate kidney function, liver values, and overall health. This is critically important because hyperthyroidism increases blood flow to the kidneys, which can mask underlying chronic kidney disease (CKD). When thyroid levels are normalized by treatment, renal blood flow decreases to its true baseline, potentially unmasking kidney insufficiency that was previously hidden. This relationship between hyperthyroidism and kidney function directly influences which treatment approach is most appropriate for each individual cat.

Treatment Options: Medications, Radioiodine, Surgery, and Diet
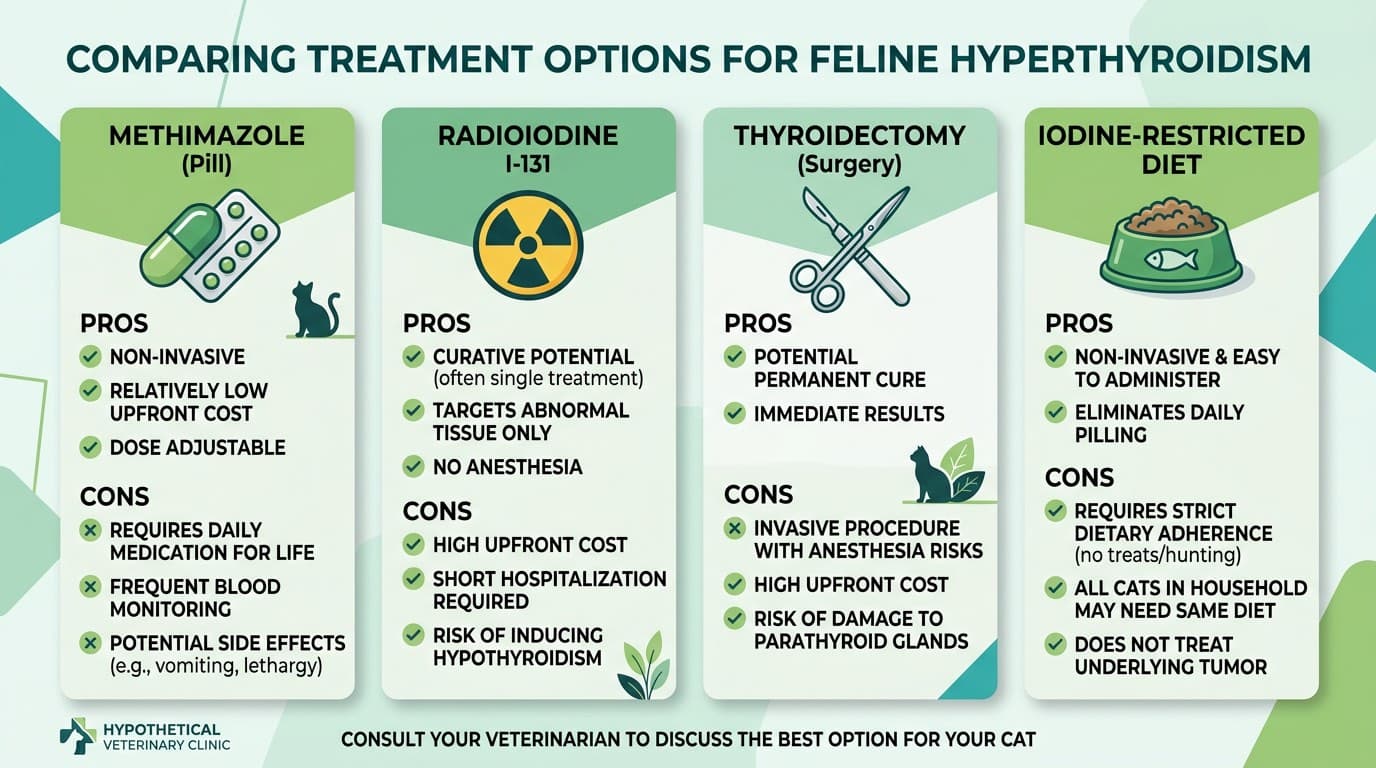
Four established treatment modalities are available for feline hyperthyroidism, and the best choice depends on the cat's overall health, the presence or absence of concurrent kidney disease, the owner's preferences and resources, and the availability of specialty services.
Methimazole (Tapazole/Felimazole) is the most commonly used medical treatment and works by blocking the thyroid gland's ability to produce hormones. It is available as an oral tablet, a flavored liquid, or a transdermal gel applied to the inner ear pinna. Methimazole does not cure the disease — it controls it — and must be administered daily for the rest of the cat's life. Most cats tolerate it well, but potential side effects include gastrointestinal upset, facial itching, and, rarely, bone marrow suppression or liver toxicity. Regular blood monitoring (every three to six months) is necessary to adjust dosing and monitor for adverse effects. Methimazole is also used as a diagnostic trial: if kidney values rise when T4 normalizes, it signals significant underlying kidney disease that would need to be factored into long-term treatment decisions.
Radioiodine therapy (I-131) is considered the gold standard treatment because it is curative in over 95 percent of cases with a single injection. Radioactive iodine is administered subcutaneously, concentrates selectively in overactive thyroid tissue, and destroys it while sparing normal thyroid cells and parathyroid glands. The procedure requires a brief hospitalization (typically three to five days) at a licensed facility until radiation levels fall below regulatory limits. There are no daily medications afterward, no anesthesia risk, and no surgical incisions. The primary barriers are cost and limited availability, as only certain veterinary centers are licensed for nuclear medicine.
Thyroidectomy (surgical removal of the affected thyroid gland) provides a definitive cure and is appropriate when radioiodine is unavailable or when the cat is a good anesthetic candidate. Risks include inadvertent damage to the parathyroid glands (causing hypocalcemia), anesthetic complications in older cats, and potential recurrence if bilateral disease is not fully addressed. Post-operative monitoring of calcium levels is essential for the first several days.
Iodine-restricted diet (Hill's Prescription Diet y/d) limits the iodine available for thyroid hormone production and can be effective when it is the cat's sole source of nutrition. This approach avoids medications and procedures entirely but requires strict dietary compliance — no treats, table food, hunting, or other pet foods. It is most practical for indoor-only cats in single-cat households where dietary control can be absolute.
The Thyroid-Kidney Connection
One of the most clinically significant considerations in managing feline hyperthyroidism is its relationship with chronic kidney disease (CKD), as both conditions are highly prevalent in senior cats and frequently coexist. Hyperthyroidism increases cardiac output and renal blood flow, which elevates the glomerular filtration rate (GFR) and can artificially improve — or mask — declining kidney function on blood work. A cat with concurrent CKD may have normal-appearing kidney values (BUN and creatinine) while hyperthyroid, but once thyroid hormone levels are normalized through treatment, the true extent of kidney compromise becomes apparent.
This phenomenon has direct implications for treatment selection. Before pursuing a permanent cure (radioiodine or surgery), most veterinarians recommend a methimazole trial period of four to six weeks. If kidney values remain stable after T4 is normalized, the cat is a good candidate for definitive treatment. If kidney values rise significantly, the cat may benefit from continuing methimazole at a dose that partially controls the hyperthyroidism while preserving enough renal blood flow to support kidney function — a carefully managed compromise known as "permissive hyperthyroidism."
Regular monitoring of both thyroid and kidney parameters is a cornerstone of long-term management. Cats on methimazole should have blood work checked every three to six months, including total T4, BUN, creatinine, SDMA (a more sensitive marker of kidney function), electrolytes, and a urinalysis. Early detection of kidney decline allows for timely dietary and therapeutic interventions, including renal diets, phosphorus binders, and subcutaneous fluid therapy, that can significantly extend quality of life.

What You Can Do at Home
Living with a hyperthyroid cat is manageable with consistent veterinary partnership and a few practical home routines. If your cat is on methimazole, establish a reliable daily medication schedule. For cats that resist pills, ask your veterinarian about transdermal methimazole gel, which is applied to the inside of the ear flap with a gloved finger and absorbed through the skin. Rotate application between left and right ears, and wipe the ear gently with a damp cloth before each new application to ensure consistent absorption.
Monitor your cat's weight at home using a baby scale or by weighing yourself holding the cat and subtracting your own weight. Record the weight weekly. Stable or increasing weight is a positive sign that treatment is working. Continued weight loss despite treatment warrants a veterinary re-evaluation of the T4 level, medication dose, or investigation for concurrent conditions. Similarly, track your cat's water intake, appetite, activity level, and litter box output — changes in any of these parameters can signal a shift in thyroid or kidney function.
Keep all scheduled follow-up blood work appointments, even when your cat appears to be doing well. Hyperthyroidism management is dynamic, and medication doses may need periodic adjustment as thyroid tissue changes over time. If your cat is on an iodine-restricted diet (y/d), strict compliance is essential — even small amounts of iodine from treats, other pet foods, or hunting can undermine the diet's effectiveness. For multi-cat households, feeding the hyperthyroid cat separately in a closed room during meal times is often the most practical solution to prevent dietary cross-contamination.

Frequently Asked Questions
What causes hyperthyroidism in cats?
In 97 to 99 percent of cases, feline hyperthyroidism is caused by a benign functional tumor called a thyroid adenoma that produces excess thyroid hormones. The exact trigger for adenoma development is not fully understood, but environmental factors such as exposure to flame retardants, certain canned food linings, and indoor-only lifestyles have been investigated as potential contributors. Thyroid carcinoma (cancer) accounts for fewer than three percent of cases.
How much does radioiodine (I-131) treatment cost for a cat?
Radioiodine therapy typically costs between $1,000 and $2,500 in the United States, depending on the facility and geographic region. This includes the radioactive iodine injection, mandatory hospitalization for three to five days while radiation levels decrease, and follow-up blood work. While the upfront cost is higher than starting methimazole, radioiodine is curative and eliminates the ongoing expense of daily medication and frequent monitoring blood tests.
Can hyperthyroidism in cats be cured?
Yes. Radioiodine therapy (I-131) cures hyperthyroidism in over 95 percent of cats with a single treatment, and thyroidectomy also provides a definitive cure in appropriate surgical candidates. Methimazole controls the disease effectively but does not cure it and must be given daily for life. The iodine-restricted diet controls thyroid hormone production only as long as it remains the cat's exclusive food source.
Why does my veterinarian want to check kidney values before treating hyperthyroidism?
Hyperthyroidism increases blood flow to the kidneys, which can mask underlying chronic kidney disease by artificially improving kidney values on blood work. When thyroid levels are normalized through treatment, renal blood flow returns to baseline, potentially revealing kidney disease that was previously hidden. A methimazole trial period allows your veterinarian to assess kidney function at a normal thyroid level before committing to a permanent treatment that cannot be reversed.
Is the iodine-restricted diet effective for treating hyperthyroidism in cats?
The iodine-restricted diet (Hill's y/d) can effectively control thyroid hormone levels when it is the cat's sole source of nutrition. However, strict compliance is essential — any treats, table food, other pet foods, or prey items containing iodine will undermine the diet's effect. It is most practical for indoor-only cats in single-pet households. Many veterinarians consider it a good option for cats that cannot tolerate medication or are not candidates for radioiodine or surgery.
References
- Peterson, M.E. "Hyperthyroidism in Cats: What's Causing This Epidemic of Thyroid Disease and Can We Prevent It?" Journal of Feline Medicine and Surgery, 2012.
- Cornell University College of Veterinary Medicine, Cornell Feline Health Center. "Hyperthyroidism in Cats." cornellcats.org, 2024.
- Merck Veterinary Manual. "Hyperthyroidism in Cats." merckvetmanual.com, 2024.
- Carney, H.C. et al. "AAFP Guidelines for the Management of Feline Hyperthyroidism." Journal of Feline Medicine and Surgery, 2016.
